Abstract
Retinitis Pigmentosa is a leading cause of severe vision loss. Retinitis Pigmentosa can present with a broad range of phenotypes impacted by disease age of onset, severity, and progression. This variation is influenced both by different gene mutations as well as unique variants within the same gene. Mutations in the nuclear hormone receptor 2 family e, member 3 are associated with several forms of retinal degeneration, including Retinitis Pigmentosa. In our previous studies we demonstrated that subretinal administration of one Nr2e3 dose attenuated retinal degeneration in rd7 mice for at least 3 months. Here we expand the studies to evaluate the efficacy and longitudinal impact of the NR2E3 therapeutic by examining three different doses administered at early or intermediate stages of retinal degeneration in the rd7 mice. Our study revealed retinal morphology was significantly improved 6 months post for all doses in the early-stage treatment groups and for the low and mid doses in the intermediate stage treatment groups. Similarly, photoreceptor function was significantly improved in the early stage for all doses and intermediate stage low and mid dose groups 6 months post treatment. This study demonstrated efficacy in multiple doses of NR2E3 therapy.
Similar content being viewed by others
Introduction
Retinitis Pigmentosa (RP) is a heterogeneous, pleiotropic group of inherited retinal diseases which affect every 1 in 4000 people and occur in syndromic and non-syndromic forms1,2,3,4,5,6,7,8,9,10. RP can occur through multiple modes of inheritance including autosomal-dominant (15–25% of cases), autosomal-recessive (5–20% of cases), X-linked (5–15% of cases), and simplex (40–50% of cases)2,6,7,11,12. Non-syndromic and syndromic forms of RP are associated with over 4300 mutations across more than 100 identified genes resulting in variable age of onset, disease progression rate, and severity depending on the specific mutations and genes impacted1,12,13,14. Despite the considerable phenotypic variation in RP, photoreceptor cell degeneration is the primary pathology identified in all types of RP. Currently, there is no cure for RP and the disease is genetically unidentifiable in approximately 50% of patients11,15.
In recent studies our lab demonstrated the novel use of nuclear hormone receptor 2 family e, member 3 (Nr2e3) as a genetic modifier and therapeutic for several forms of RP in multiple mouse models including rd716. Treatment of each RP mouse model with a subretinal injection of Nr2e3 resulted in stabilized retinal function, preserved retinal morphology, increased photoreceptor survival, and altered expression in several genes and transcription factors associated with biological pathways involved in maintaining retinal homeostasis and development. The study demonstrated improvements at the functional, histological, and immunohistochemical level of 30–80% in all RP models. Nr2e3 was shown to be expressed in the regions of rescue in treated retinas. The study by Li et al. also investigated the mechanism of Nr2e3 rescue via changes in gene expression in 8 Nr2e3-directed networks involved in maintaining retinal homeostasis: apoptosis, ER stress, immunity, metabolism, neuroprotection, oxidative stress, phototransduction, and cell survival. Several genes in each of these networks were differentially expressed following Nr2e3 treatment in rd7 mice indicating the involvement of Nr2e3 in modulating networks involved in retinal homeostasis16. Our present study builds on the findings of Li et al. by examining efficacy of three different NR2E3 GLP quality doses, extending the longitudinal observation time to 6 months after NR2E3 administration, and examining treatment during early and intermediate stages of disease progression in order to inform clinical trials.
NR2E3 is a nuclear hormone receptor expressed in retinal progenitors, rods, and cones17,18, and as such plays a pivotal role in modulating several biological pathways essential for maintaining homeostasis in the retina including apoptosis, cell survival, ER stress, immunity, metabolism, neuroprotection, oxidative stress, and phototransduction16. NR2E3 associated retinal diseases include several recessive diseases: clumped pigmentary retinal degeneration (CPRD), enhanced S-cone syndrome (ESCS), Goldmann–Favre syndrome (GFS), and autosomal dominant Retinitis Pigmentosa (adRP)19,20,21,22,23,24,25,26,27. GFS and CPRD patients with NR2E3 mutations share some clinical phenotypes common in ESCS such as night blindness, reduced rod function, and hyper S-cone function25,28. ESCS in humans is characterized by an increase in S (short, blue) cone photoreceptor function along with degeneration in rods and red and green cones that results in blue light sensitivity, night blindness and vision loss23,29,30,31,32,33,34. GFS is a vitreoretinal degenerative disease, considered to potentially be a milder form of ESCS, that presents with cystoid macular edema (CME), foveal and peripheral retinoschisis, night blindness, pigmentary degeneration, and vitreous changes28,35,36. CPRD is characterized by typical RP symptoms accompanied by accumulation of melanin granules in the retinal pigment epithelium (RPE) resulting in large pigment deposits in the peripheral retina25,37,38. The correlation of NR2E3 with various disease phenotypes and modes of inheritance strongly suggests that these degenerative diseases likely develop on a permissive or selective genetic background and are likely influenced by the specific mutations as well as modifier genes16,20,22,24,39.
Adeno-associated viruses (AAVs) have proven to be effective therapeutic gene delivery vectors for treating diseases such as inherited retinal degeneration due to their variability in cell type specificity, long term expression and low immune response40,41,42,43,44,45,46,47. Adeno-associated virus serotype 5 (AAV5) containing the human NR2E3 gene (AAV5-hNR2E3) was chosen as the viral vector for this study based on our previous study that examined AAV2.7m8, AAV5, and AAV8 gene delivery16 along with several safety and efficacy studies40,41,44. AAV5 transduces RPE and photoreceptor cells more efficiently and in greater volumes than other AAVs, especially AAV240,41,42. Studies also showed that AAV5 has a low immunogenic response in humans due to their low numbers of pre-existing circulating AAV5 antibodies44.
This is a pharmacological preclinical longitudinal study of the dose–response and efficacy of subretinal delivery of AAV5-hNR2E3 to ameliorate and attenuate retinal degeneration when administered during early (postnatal day (P) 30) or intermediate (3-months of age) disease progression in the RP mouse model rd7 1, 3, and 6 months after treatment. The Nr2e3rd7/J (rd7) mouse is a model for recessive NR2E3-associated retinal disease18,48,49,50. The rd7 mouse exhibits bilateral pan retinal spots observed at eye opening (P14) which fade with degeneration, and whorls and rosettes in the outer nuclear layer (ONL) of the retina that are apparent histologically by P1016,18,50. As the phenotype progresses, a flattening of whorls and reduction of retinal spots is observed around 5 months of age followed by progressive loss of the ONL and outer segment thickness and appearance of mottled retinal pigment by 16 months of age50. Also, electroretinogram levels do not fall below normal until about 5 months of age and are reduced by approximately 50% by 16 months of age50. There are two components of disease in rd7 mice: a developmental problem in the retinal progenitors resulting in abnormal increase in blue opsin expressing cone cells due to over proliferation of cone cells (not at the expense of other cell types such as rods), followed by a slow and progressive degeneration of cone and rod photoreceptor cells18,50. The results of this study showed that administration of AAV5-hNR2E3 at any of the three doses evaluated resulted in sustained attenuation of retinal degeneration over 6 months when administered during early or intermediate progression of rd7 retinal degeneration.
Results
Subretinal delivery of three doses of AAV5-hNR2E3 in rd7 mice during early or intermediate disease stages shows no adverse effects on the clinical phenotype
The long-term effects of NR2E3 on the clinical phenotype of rd7 animals were evaluated following subretinal delivery of AAV5 during early or intermediate stages of rd7 clinical disease progression. Animals were treated with either a low, mid, or high dose of AAV5-hNR2E3 at P30 or 3 months of age, and evaluated 1-, 3-, and 6-months post treatment to monitor for any longitudinal adverse effects of NR2E3 on the rd7 animals. The rd7 fundus phenotype has pan retinal spots that lack a consistent spatial or numerical pattern; with variability in the density of spots. These spots fade as degeneration progresses; thus, while it is not useful to quantify the number of retinal spots, the fundus can be used to qualitatively evaluate potential signs of gross abnormalities or inflammation due to treatment, such as retinal scarring, by comparing treated eyes with uninjected and mock injected eyes. Early-stage fundus analysis of rd7 animals treated with NR2E3 at P30 revealed no long-term negative effects such as an increase in pan retinal spots or inflammation in the fundus phenotype for all doses (Fig. 1). Similarly, longitudinal monitoring of intermediate stage treatment (rd7 animals treated at 3-months of age) with NR2E3 revealed no gross abnormalities in the fundus phenotype for all three therapeutic doses (Fig. 2). OCT was performed to track in life observation of any potential adverse effects. No adverse effects were observed in 1-, 3-, and 6-month post early stage (Fig. 1B) and intermediate stage (Fig. 2B) NR2E3 treated rd7 mice. Microglial cells are the main constituents of the immune cell population in the retina and the main initiators of the inflammatory response in the retina51,52,53,54. Our prior studies showed that rd7 mice do not undergo inflammation17. In order to determine if AAV5-hNR2E3 treatment will induce an inflammatory response through microglial activation, we examined the expression of IBA1, a marker of microglial activation. The results show that there is no evidence of microglial activation reflecting absence of inflammation in NR2E3-treated rd7 mice, similar to normal B6 and untreated rd7 mice (Supplemental Fig. S1).
Treatment during early disease in rd7 mice with low, mid, and high dose NR2E3 showed no adverse effects on the clinical phenotype. (A) Fundus of C57BL6/J (B6) wild-type and untreated rd7 animals used for pre-treatment and age matched controls, and (B) rd7 animals injected at P30 with low, mid, and high dose NR2E3 and assessed 1-, 3-, and 6-months post injection (animal ages 2, 4, and 7 months). (B) Optical coherence tomography of 1 month old wild-type C57BL6/J (B6), and untreated rd7 mice as pre-treatment controls (upper panels). rd7 animals dosed at P30 and assessed 1-, 3-, and 6-months post injection (animal ages 2, 4, and 7 months), and age matched untreated rd7 controls (lower panels). Arrows indicate whorls and rosettes. All images were collected at approximately the same location at the central retina. Low Dose = 1 × 108 v/gc, Mid Dose = 1 × 109 v/gc, and High Dose = 4 × 109 v/gc. n ≥ 5.
Low, mid, and high dose NR2E3 treatment in rd7 mice during intermediate degeneration revealed no adverse effects on clinical phenotype. (A) Fundus of C57BL6/J (B6) wild-type and untreated rd7 animals used for pre-treatment and age matched controls, and (B) rd7 animals injected at 3-months of age with low, mid, or high dose NR2E3 and assessed 1-, 3-, and 6-months post injection (animal ages 4, 6, and 9 months). (B) Optical coherence tomography of (A). 3-month-old wild-type C57BL6/J (B6), and untreated rd7 mice as pre-treatment controls (upper panels). rd7 animals dosed at 3-months of age and assessed 1-, 3-, and 6-months post injection (animal ages 4, 6, and 9 months), and age matched untreated rd7 controls (lower panels). Arrows indicate whorls and rosettes. All images were collected at approximately the same location at the central retina. Low Dose = 1 × 108 v/gc, Mid Dose = 1 × 109 v/gc, and High Dose = 4 × 109 v/gc. n ≥ 5.
AAV delivery of NR2E3 in different doses in rd7 animals during early or intermediate disease progression restores retinal morphology
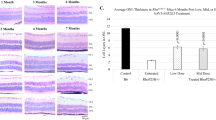
Histology analysis of rd7 animals dosed with AAV5-hNR2E3 during early or intermediate disease progression showed improved retinal morphology. rd7 mice exhibit a slow, progressive, concomitant degeneration of rod and cone photoreceptors, leading to resolution of the whorls over time. A normal mouse retina consists of 10–12 layers of cone and rod photoreceptor nuclei making up the ONL and 5–6 layers of inner retinal cells making up the inner nuclear layer (INL)16. In the rd7 model, abnormal morphology presents with whorls and rosettes in the ONL caused by over-proliferation of blue opsin expressing cone cells followed by slow, progressive photoreceptor degeneration18,50. The whorls and rosettes begin to resolve and flatten by 5 months of age as degeneration progresses50. The non-whorl regions of the retina are the most important for tracking degeneration and rescue as abnormal blue cone proliferation has not disrupted the normal thickness of this region prior to disease onset. Hematoxylin/Eosin (H/E) staining showed fewer whorls and rosettes and increased ONL thickness in P30 treated retinas for all doses over 6 months compared to untreated retinas (Fig. 3, lower magnification in Supplemental Fig. S2). H/E analysis of rd7 animals treated with NR2E3 at 3-months of age similarly demonstrated a reduction in whorls and rosettes and increased ONL thickness in treated retinas for all doses compared to untreated maintained over 6 months (Fig. 4). Some whorls and rosettes will still be present in treated retinas if they were present prior to NR2E3 administration halting proliferation and degeneration. Additionally, to discern the impact of rescue, the ONL in the non-whorl and rosette regions of rd7 animals treated at P30 or 3-months of age and collected 6-months after treatment were counted and compared with untreated retinas. Statistically significant rescue of photoreceptor cells in the non-whorl regions was observed compared to untreated animals in both early and intermediate administration groups except for the intermediate stage high dose treatment (Fig. 5; p < 0.05 to 0.0001). Both the P30 and 3-month injected low dose groups rescued similar amounts of photoreceptors. Interestingly, animals treated at P30 showed rescue to normal ONL thickness (around 10–12 layers) for all doses, compared to mid and high dose animals treated at 3-months of age that showed a more modest rescue of around 8–9 layers. This is likely due to degeneration already occurring when treatment was administered at the intermediate progression phase (3-months of age) and thus fewer cells remained that could be rescued. These data suggest that NR2E3 is effective at halting degeneration when administered at early or a later stage of disease for all doses except the high dose later stage, and for at minimum 6 months after treatment.
AAV5-hNR2E3 treatment at P30 rescues retinal morphology in rd7 retinas in low, mid, and high doses. (A) C57BL6/J (B6) 1-, 3-, and 6-month wild-type H/E. (B) rd7 animals injected at P30 and collected 1-, 3-, and 6-months post injection (animal ages 2, 4, and 7 months) with low, mid, or high dose therapy, and age matched untreated rd7 controls. White boxes on the 7-month images indicate where cell counts were performed representatively. Low Dose = 1 × 108 v/gc; Mid Dose = 1 × 109 v/gc, High Dose = 4 × 109 v/gc. GCL Ganglion Cell Layer, INL Inner Nuclear Layer, ONL Out Nuclear Layer. Scale bar = 50 µm. n ≥ 5.
AAV5-hNR2E3 treatment during intermediate disease rescues retinal morphology in rd7 retinas in low, mid, and high doses. (A) C57BL6/J (B6) 3-, 6-, and 12-month wild-type H/E. (B) rd7 animals injected at 3-months of age and collected 1-, 3-, and 6-months post injection (animal ages 4, 6, and 9 months) with low, mid, or high dose therapy, and age matched untreated rd7 controls. White boxes on the 9-month images indicate where cell counts were performed representatively. Low Dose = 1 × 108 v/gc; Mid Dose = 1 × 109 v/gc, High Dose = 4 × 109 v/gc. GCL Ganglion Cell Layer, INL Inner Nuclear Layer, ONL Out Nuclear Layer. Scale bar = 50 µm. n ≥ 5.
AAV5-hNR2E3 treatment reduces ONL degeneration from disease progression in rd7 animals at all doses. Outer nuclear layer (ONL) thickness of animals injected at P30 (early) or 3-months of age (intermediate) and collected 6-months post injection (animal ages 7 months and 9 months) were compared with the non-whorl region of untreated rd7 animals of the same age. Early AAV5-hNR2E3-treated rd7 animals untreated vs low dose p < 0.006, untreated vs mid dose p < 0.0001, untreated vs high dose p < 0.009. Intermediate AAV5-hNR2E3-treated rd7 animals untreated vs low dose p < 0.0001, untreated vs mid dose p < 0.04; low dose vs mid dose p < 0.02; low dose vs high dose p < 0.002. Dots represent individual data points for each experimental group. Serial section of central retina counted over 100 µm. Low Dose = 1 × 108 v/gc; Mid Dose = 1 × 109 v/gc, High Dose = 4 × 109 v/gc. Results are mean ± SEM, n ≥ 5.
Cone and rod opsin expression is preserved in rd7 animals treated during early or intermediate stage progression with AAV5-hNR2E3 dose therapy
Immunohistochemical analysis was performed to examine the efficacy of three different doses of AAV5-hNR2E3 to evaluate blue and green cone opsin and rhodopsin expression in rd7 mice. Our previous studies demonstrated that untreated rd7 animals exhibit an increase in blue opsin expression followed by slow progressive loss of blue and green opsin and rhodopsin expression with disease progression over 5–16 months16,18. Animals treated with AAV5-hNR2E3 at P30 showed preserved expression of all opsins compared to untreated animals for the low, mid, and high doses that was sustained to 6-months post treatment, assessed using green and blue opsin-positive cell counts and mean fluorescence intensity of the three opsins (p < 0.05 for all doses) (Fig. 6). Similarly, rd7 mice treated with NR2E3 at 3-months of age had preserved opsin expression sustained over 6 months after treatment for all doses, which was assessed using opsin cell counts and mean fluorescence intensity of the opsins (p < 0.05 for the low and mid doses for opsin counts) (Fig. 7). IHC analysis also supports our histological findings of partial rescue and restored retinal morphology from focal delivery of NR2E3 dose treatment. All three doses showed rescue with no gross abnormalities or remarkable loss of expression of rod or cone opsins.
AAV5-hNR2E3 treatment during early disease preserves opsin expression and restores retinal morphology in rd7 mice at low, mid, and high doses. Immunohistochemical analysis of opsin expression in rd7 animals treated with low, mid, and high dose NR2E3 at P30 and collected 1-, 3-, and 6-months post treatment (animal ages 2, 4, and 7 months). (A) Green opsin (OPN-MW), (B) blue opsin (OPN-SW), and (C) rhodopsin (RHO) expression in treated and untreated animals for all doses and collection times. (D) C57BL6/J (B6) wild-type green opsin, blue opsin, and rhodopsin controls. (E,F) Green and blue opsin-positive cell counts in early NR2E3 treated 6 months post rd7 mice. Green opsin counts untreated vs low dose p < 0.0006, untreated vs mid dose p < 0.0001, untreated vs high dose p < 0.0001. Blue opsin counts untreated vs low and mid doses p < 0.04, untreated vs high dose p < 0.007. (G–I) Mean fluorescence intensity of green opsin, blue opsin, and rhodopsin in early NR2E3-treated 6 months post rd7 mice. Green opsin intensity untreated vs low dose p < 0.05, untreated vs mid dose p < 0.03, untreated vs high dose p < 0.005. Blue opsin intensity untreated vs low dose p < 0.007, untreated vs mid and high doses p < 0.009. Rhodopsin intensity untreated vs low dose p < 0.03, untreated vs mid dose p < 0.005, untreated high dose p < 0.03. DAPI staining depicted in blue. Opsin shown in green. Low Dose = 1 × 108 v/gc; Mid Dose = 1 × 109 v/gc, High Dose = 4 × 109 v/gc. Scale bar = 50 µm. Results are mean ± SEM, n ≥ 5.
AAV5-hNR2E3 treatment during intermediate disease preserves opsin expression and restores retinal morphology in rd7 mice at low, mid, and high doses. Immunohistochemical analysis of opsin expression in rd7 animals treated with low, mid, and high dose NR2E3 at 3-months of age and collected 1-, 3-, and 6-months post treatment (animal ages 4, 6, and 9 months). (A) Green opsin (OPN-MW), (B) blue opsin (OPN-SW), and (C) rhodopsin (RHO) expression in treated and untreated animals for all doses and collection times. (D) C57BL6/J (B6) wild-type green opsin, blue opsin, and rhodopsin controls. (E,F) Green opsin-positive cell counts and blue opsin-positive cell counts in intermediate NR2E3 treated 6 months post rd7 mice. Green opsin counts untreated vs low dose p < 0.004, untreated vs mid dose p < 0.007. Blue opsin counts untreated vs low dose p < 0.004, untreated vs mid dose p < 0.04. (G–I) Mean fluorescence intensity of green opsin, blue opsin, and rhodopsin in intermediate NR2E3-treated 6 months post rd7 mice. Green opsin intensity untreated vs low dose p < 0.02, untreated vs high dose p < 0.05. Blue opsin intensity untreated vs low dose p < 0.009, untreated vs mid dose p < 0.05. Rhodopsin intensity untreated vs low dose p < 0.02, untreated vs high dose p < 0.04. DAPI staining depicted in blue. Opsin shown in green. Low Dose = 1 × 108 v/gc; Mid Dose = 1 × 109 v/gc, High Dose = 4 × 109 v/gc. Scale bar = 50 µm. Results are mean ± SEM, n ≥ 5.
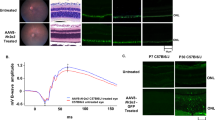
AAV5-hNR2E3 improved scotopic ERG responses in rd7 animals treated during early or intermediate progression
The rd7 mice exhibit progressive loss of rod and cone function as measured by abnormal ERG responses with significant loss of function between 6–12 months of age18,50,55. Our previous studies of rd7 mice treated with Nr2e3 showed improved ERG responses measured up to 3-months post treatment16,18. In this study, dark-adapted and light-adapted ERGs were used to assess photoreceptor function of treated rd7 retinas by examining rod- and cone-driven responses up to 6-months post treatment (Fig. 8A–D; Supplemental Fig. S3). Similarly to cell counts, rd7 animals treated during early stage (P30) progression demonstrated statistically significant rescue of dark-adapted photoreceptor function in low, mid and high dose treated retinas (p < 0.0001 for all doses) compared to untreated 6 months post treatment (Fig. 8A). rd7 mice treated at intermediate stage (3-months of age) of disease only showed significant rescue 6-months post treatment for the low and mid dose groups compared to untreated retinas (Fig. 8A, p < 0.0001). A significant improvement in the dark-adapted a-wave function and light-adapted b-wave function was also observed in early and intermediate mid dose treated rd7 retinas compared with untreated retinas (Fig. 8B,C). Significant improvement in photoreceptor function was often not detectable until 6-months post treatment for both administration time points; this could be attributed to the delay in expression of AAV5-hNR2E342,56. The appearance of improved function and lack of significance for some of the doses and time points could be affected by technical aspects of delivery and measuring function via ERG. The focal delivery of NR2E3 via subretinal injection will only rescue a localized portion of the retina whereas full-field ERG measures overall photoreceptor function across the entire retina. The different levels of rescue observed in ERGs for each of the doses and time points is the result of the varying amounts of rescue achieved by localized delivery. Interestingly, animals injected at P30 showed increased improvement in ERG response over time for all doses, perhaps supporting the idea that earlier therapeutic intervention has a chance of improving clinical outcome.
AAV5-hNR2E3 improved peak scotopic b-wave amplitude in rd7 mice for all doses. C57BL6/J (B6) animals were used for wild-type controls. (A) The scotopic b-wave amplitudes of rd7 animals injected at P30 were assessed 1-, 3-, and 6-months post injection for the low, mid, and high dose (animal ages 2, 4, and 7 months). rd7 animals injected at 3-months of age were similarly assessed 1-, 3-, and 6-months post injection for the low, mid, and high dose (animal ages 4, 6, and 9 months). Treated eyes showed significant improvement of retinal function at the 6-month post-injection time points for both the 1 month-injected low and mid dose groups and 3 month-injected mid dose group when compared with age-matched untreated eyes. Intermediate AAV5-hNR2E3 treated 3 months post rd7 mice untreated vs mid dose p < 0.05. Early AAV5-hNR2E3 treated 6 months post rd7 mice untreated vs low dose p < 0.003, untreated vs mid dose p < 0.0001 and untreated vs high dose p < 0.02. Intermediate AAV5-hNR2E3 treated 6 months post rd7 mice untreated vs low dose p < 0.03 and untreated vs mid dose p < 0.0001; low vs mid dose p < 0.04, and mid vs high dose p < 0.0002. Dots represent individual data points for each experimental group. (B) The scotopic a-wave amplitudes of rd7 mice receiving early or intermediate NR2E3 treatment. Early NR2E3 treated 6M post rd7 mice untreated vs mid dose p < 0.009. Intermediate NR2E3 treated 6M post rd7 mice untreated vs mid dose p < 0.003 and mid dose vs high dose p < 0.02. (C) The photopic b-wave amplitudes of early and intermediate NR2E3-treated rd7 mice assessed at 1, 3 and 6 months post-treatment. Early NR2E3 treated 6M post rd7 mice untreated vs mid dose p < 0.002. Intermediate NR2E3 treated 6M post rd7 mice untreated vs mid dose p < 0.007 and mid dose vs high dose p < 0.005. (D) The photopic a-wave amplitude of early and intermediate NR2E3 treated rd7 mice at 1, 3 and 6 months post-treatment. Low Dose = 1 × 108 v/gc; Mid Dose = 1 × 109 v/gc, High Dose = 4 × 109 v/gc. Results are mean ± SEM. n ≥ 5.
Discussion
The outcomes of inherited diseases such as RP are subject to the influence of several factors including allelic heterogeneity, environment, epigenetic factors, and gene mutations57,58,59,60. Nr2e3 is a powerful nuclear hormone receptor that modulates several key gene networks important for maintaining homeostasis in the retina including apoptosis, cell survival, ER stress, immunity, metabolism, neuroprotection, oxidative stress, and phototransduction16,61. Our recent study demonstrated that administering Nr2e3 gene therapy prior to disease onset or during early disease rescues degeneration in the rd7 mouse model which has an Nr2e3-associated gene mutation16. This current study was a pharmacological preclinical study that informs dose selection and longitudinal effectiveness of NR2E3 therapeutic. The novel focus of this study was to examine the efficacy and longitudinal effects of dosage and early versus intermediate therapeutic intervention. All doses showed improvement of photoreceptor survival, and retinal function as well as partial restoration of retinal structure. Furthermore, no gross abnormalities were observed with any of the doses. Sustained improvement was observed up to 6 months after treatment in early and intermediate disease stage groups. It is important to note that focal delivery of NR2E3 via sub-retinal injection does not rescue the entire retina and manifests as regions of rescue localized around the injection site. This is demonstrated in the functional, histological, and molecular analysis. Localized rescue of photoreceptors illustrate why statistically significant improvements in retinal morphology were observed compared to more limited significance in full field ERGs that measures function across the entire retina. ERGs are also very technically sensitive, and variation demonstrated by the error bars is likely a result of different personnel performing the experiments. Additionally, that it can take AAVs up to 2–4 weeks to begin showing expression likely contributes to the observations of statistically significant improvements after 6 months irrespective of disease stage at time of administration42,56.
The rd7 mouse is a functional null representing varied phenotypes of recessive NR2E3-associated retinal disease that encompasses both RP and ESCS18,19,23,26,50. The rd7 mouse is unique in that it has two distinct phenotypes: a developmental over-proliferation of blue cones followed by a slow progressive degeneration of all photoreceptors. It is important to note, rd7 mice, unlike many other RP models, actually start with relatively normal expression of rhodopsin that degenerate over time along with cones. It has been suggested that rd7 mice possess some hybrid photoreceptor cells that co-express blue opsin and rhodopsin62,63; however, our prior studies could not confirm these findings nor did we observe any similarities between our individually labeled IHCs from this study (Supplemental Fig. S4)17,64. Regardless, rd7 mice have a developmental problem of over-proliferation of blue opsin expressing cone cells due to lack of Nr2e3 in retinal progenitors17. Once matured, rd7 photoreceptor cells degenerate, and that is likely due to disruption of Nr2e3 function in many pathways associated with normal function of rod and cone photoreceptor cells. The mechanism of disease in rd7 thus involves the lack of functional Nr2e3 protein that disrupts progenitor cell proliferation, rod and cone differentiation, and rod and cone function and survival17,18.
Our work and the work of others demonstrates that NR2E3 plays a role in both the developing and adult retina as well as functions as either an activator or repressor in different photoreceptor development stages17,64,65. Nr2e3 targets genes involved in key homeostasis pathways like cell survival, apoptosis, phototransduction, immunity, neuroprotection, ER stress, oxidative stress, metabolism, and immunity which could be a contributor to the degeneration of rods and cones following blue cone over-proliferation in rd7 mice when Nr2e3 proteins are nonfunctional16. Importantly, our recent studies show that many RP models have little to no expression of key retinal transcription factors (including Nr2e3. CRX, Nrl, Rora, Nr1d1) and are reset by NR2E3 therapy16. Taking the rd7 disease phenotypes into consideration, and as we treated post photoreceptor development (P30 or 3 months). NR2E3, like all NHRs, regulates multiple genes in pathways impacting cell homeostasis66,67,68, as demonstrated in our prior study16. In the current study, the mechanism of NR2E3 rescue of retinal degeneration in rd7 is likely occurring similarly through modulation of the Nr2e3 regulated genes and gene networks to a more homeostatic state that attenuates degeneration16,17,23,64.
As expected, earlier treatment of rd7 mice with NR2E3 is more effective at alleviating or ameliorating disease progression. Treatment during early disease state showed better sustained rescue over time and was able to return ONL thickness and ERG responses to normal levels. It is imperative to note that NR2E3 is a promising treatment for early or intermediate stage degeneration meaning that it can be used to treat early-stage diagnosis patients and patients that have already been diagnosed and progressed to the later stages of degeneration, which is uncommon for many therapeutics. NR2E3 was also able to provide rescue for at least 6 months in both progression stage treatments and rescued photoreceptor survival and function to near normal levels in the intermediate stage.
In conclusion, this study demonstrates that AAV5-hNR2E3 in various doses can treat early and intermediate stage retinal degeneration in the rd7 mouse for at least 6 months. The results reveal that NR2E3 gene therapy in the retina can halt degeneration and improve photoreceptor survival and function. Future studies will evaluate whether NR2E3 reverses degeneration and efficacy of combination therapies. Further studies will also investigate the effectiveness of NR2E3 therapeutic in other non-NR2E3-associated retinal diseases. The results of this pharmacology study are translational to dosage selection of NR2E3 as a therapeutic agent, longitudinal therapeutic effectiveness, and treatment effectiveness in early and intermediate stage NR2E3-associated retinal disease in clinical trials. Following this study, clinical trials of AAV5-hNR2E3 were initiated and are currently underway to examine the safety and efficacy of the therapeutic for treating various forms of Retinitis Pigmentosa and Leber Congenital Amaurosis (ClinicalTrials.gov Identifier: NCT05203939).
Materials and methods
Animal maintenance
This study was carried out in strict accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals of the National Institute of Health, as well as the Association for Research in Vision and Ophthalmology (ARVO) Statement for the Use of Animals in Ophthalmic and Vision Research. All authors complied with the guidelines for Animal Research: Reporting of In Vivo Experiments (ARRIVE). Animals were housed and bred under standard conditions, temperatures within 68–74°F and 12-h light/12-h dark cycles, in the Schepens Eye Research Institute vivarium for the duration of this study. The Schepens Eye Research Institute Animal Care and Use Committee (Protocol Number: 2020N000178) approved animal use and procedures for this study in compliance with the Animal Welfare Act Regulations. C57BL6/J (B6; Jax stock #000664), and Nr2e3rd7/J (rd7; Jax stock #002139) mice were ordered from Jackson Laboratories, Bar Harbor, ME.
Scientific rigor and reproducibility
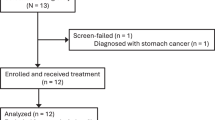
G*Power software analysis was used to conduct a power calculation for estimating the required sample size for each analysis described (G*Power, version 3.1, https://www.psychologie.hhu.de/arbeitsgruppen/allgemeine-psychologie-und-arbeitspsychologie/gpower). Based on means and standard deviation previously defined in published studies, a minimum of 4 animals were used per experimental group to provide 90% power and 30% difference at a significance level of 0.05. Every procedure was performed using a standardized protocol. This study was performed by several trained individuals in a double blinded and randomized manner to prevent any bias. At least 4–5 biological replicates were studied for each dose and time point to achieve statistical significance. Animals with cataracts, unresolved surgical trauma, or that died prematurely were excluded from the study. Based on these criteria, approximately 20% of the 120 treated animals in this study were excluded from the final analysis. Males (~ 47.37%) and females (~ 52.63%) were used equally, and a gender bias was not observed.
Statistical analysis
Graphs were analyzed for statistical significance using a two way analysis of variance (ANOVA) (GraphPad Prism, version 9.0, https://www.graphpad.com/). Comparisons were made between the mean peak scotopic or photopic a- or b-wave amplitudes of untreated and treated animals for each treatment and collection time point. Analysis of the differences between the 6-month post time point histological and opsin-positive cell counts, and mean fluorescence intensity of opsins was also performed for each dose compared to the untreated group (Supplemental Tables S1–S10).
Genotyping
Mouse tail biopsy samples were used for DNA isolation using a quick lysis sodium hydroxide method. Isolated DNA samples were amplified using the primers nr4F: GTAGCCTCTCCTGCTCTGGCAG and rd7del4R: CAGGTTGGAAAACACAGGCAAG18. For PCR amplification approximately 35 ng of DNA was used in a 10 μl reaction volume containing 10× buffer with MgCl2, 40 mM dNTP mix, 10 μM each of forward and reverse primer, and 5 U/ml AmpliTaq DNA polymerase. Reactions were denatured at 95 °C for 3 min followed by 30 cycles at 95 °C for 30 s, 60 °C for 30 s, 72 °C for 42 s and a final extension at 72 °C for 5 min. Amplicons were separated using a 2% agarose gel and visualized under UV light after staining with ethidium bromide. The wild-type amplicon is 339 base pairs (bp) in size and the mutant amplicon is 239 bp. As the rd7 mutation is a 9 kb line element insertion in the region amplified, it will not produce an Nr2e3 PCR amplicon under these conditions, and the amplicon from rd7 mice is a pseudogene18,49.
AAV5-hNR2E3 dose preparation
The drug product consists of adeno associated virus 5 (AAV5) vector containing the human NR2E3 gene (AAV5-hNR2E3 driven by the CAG promoter). The GLP vector drug product was provided by Ocugen, INC. in three different concentrations (2 × 1011 Vg/ml, 2 × 1012 Vg/ml, 8 × 1012 Vg/ml) diluted with formulation buffer (sterile solution containing 10 mM sodium phosphate, 180 mM sodium chloride, and 0.001% Poloxamer 188 (PF-68) at pH 7.3 ± 0.5). Upon arrival, the three concentrations were diluted into a low (1 × 108 vg/eye), medium (1 × 109 vg/eye), and high (4 × 109 vg/eye) dose.
Subretinal injection
AAV5-hNR2E3 was delivered by subretinal injection into the right eye of rd7 mice. Mice were injected at either P30 to treat early-stage disease progression or 3-months of age to treat intermediate progression. Control injections consisted of no injection in the contralateral (left) eye, and mock injection in the contralateral eye with saline buffer (Supplemental Fig. S5). Adults aged to P30 or 3 months old were anesthetized by intraperitoneal (IP) injection using a ketamine/xylazine mixture. A sterile 30G needle was used to make an incision in the sclera just posterior to the limbus, and a Hamilton syringe with a blunt 33G cannula attached was inserted into the incision16. A total volume of 0.5 µl of therapeutic product was manually injected into the subretinal space of the adult mice for each dosage group: low (1 × 108 vg/eye), medium (1 × 109 vg/eye), and high (4 × 109 vg/eye) dose. Accessing the central retinal region with an injection in the mouse is difficult. Therefore, the location of rescue often appeared between the peripheral and central retina, sometimes extended into the central retina based on the degree of rescue achieved by the focal injection.
Clinical examination
All animals (treated, untreated, wildtype (WT) B6 controls) underwent fundus examination and optical coherence tomography (OCT). Animals were anesthetized with a ketamine/xylazine mixture by IP injection and 1% tropicamide was used to dilate pupils. The Micron III Retinal Imaging Camera (Phoenix Research Laboratories, Pleasanton, CA, USA) and Stream Pix software (version 5, https://www.norpix.com/products/streampix/streampix.php) were used for fundus imaging. The Bioptigen OCT scanner (Bioptigen Inc, Durham, North Carolina, USA) and software (Envisu Invivovue, version 2, https://www.leica-microsystems.com/products/surgical-microscopes/p/envisu-r-class/) were used to perform OCT. A mounting tube with a bite bar restrained mice while the real time OCT image was used for alignment of the retina. Each eye had four rotational cross section scans (nasal-caudal and dorsal–ventral) taken with 100 series/scan18. The Bioptigen OCT software analyzed the retinal scans and representative images were taken of the central retina near the optic nerve.
Electroretinography
Mice were examined through electroretinography analysis as previously described16,17. Animals were dark-adapted overnight or for a minimum of 4 h before being anesthetized. Anesthesia was administered through an IP injection of a mixture of ketamine and xylazine, and pupils were dilated with 1% tropicamide. Genteal was used as a lubricant to prevent cataracts forming during the procedure. The reference electrode was placed subcutaneously in the forehead and the ground electrode was inserted subcutaneously in the tail base. Gold loop electrodes (Diagnosys LLC) were placed on the corneal apex. The Espion Visual Electrophysiology System (Diagnosys LLC, Lowell, MA, USA) performed dark- and light-adapted ERGs. Dark- and light-adapted responses were recorded according to the same protocol used previously16. Briefly, responses were recorded at intensities between 0.000249 and 24.1 cd s/m2 in 4.0 log intensity increments for dark-adapted. Using the same 4.0 log intensity difference, light-adapted responses were obtained between 0.1 and 25.6 cd s/m2 following 7 min of adaptation to background light. The peak a- and b-wave amplitude from each treated animal was selected between intensities of 0.061 cd s/m2 and 24.1 cd s/m2 for scotopic responses and 0.1 cd s/m2 and 25.6 cd s/m2 for photopic responses, averaged for each dose and time point, and plotted in comparison to peak amplitudes from wild type and untreated rd7 mice.
Histology
Histological analysis was performed as previously described16. Directly following euthanasia, a cautery mark was made on the eyes for dorsal orientation and then eyes were enucleated. Tissues from AAV5-hNR2E3 treated animals were immediately immersed in 4% paraformaldehyde (PFA) diluted with 1× phosphate buffered solution (PBS) and left overnight at 4 °C. Untreated tissue was immersed in 4% PFA and similarly left overnight at 4 °C. Eyes were paraffin embedded the following day with dorsal/ventral orientation using the cautery mark made after euthanasia. Embedded eyes were trimmed in the sagittal plane to a depth of 100 µm. 5 µm serial sections were collected at about 100 µm of retinal depth. Deparaffination of retina sections was performed in xylene and ethanol washes followed by staining with hematoxylin and eosin Y. Stained sections were mounted with Permount mounting medium16. Visualization of the rescued regions and image capture of the slides was performed with the Leica DMI6000 microscope (Leica Microsystems, Wetzlar, Germany). Identification of the rescued regions was performed visually prior to image captures to ensure that images were of the rescued regions. Cell counts were accomplished in a double-blinded manner with at minimum three individuals. Cell layer number in the outer nuclear layer (ONL) was counted for treated and untreated samples and B6 control samples. In untreated samples, cell layer counts were done for non-whorl regions of the retina. Percent observed rescue was quantified by comparing ONL cell layer numbers in treated samples to untreated and B6 control ONL counts.
Immunohistochemistry
Immunohistochemistry (IHC) analysis was performed on 5 µm retinal serial sections from the same tissue samples used for histology staining previously described. Tissue sections were blocked for 1 h with 2% normal horse serum (S-2000 Vector Labs, CA) in 1× PBS then, incubated overnight in a 1:200 dilution of the following cell type-specific primary antibodies: blue opsin (rabbit polyclonal, Millipore AB5407); green/red opsin (rabbit polyclonal, Millipore AB5405); and rhodopsin (mouse monoclonal, Millipore MAB5356). On the second day, sections were rinsed with 1X PBS and incubated for 1 h in the dark in a 1:400 dilution of the following corresponding secondary antibodies: mouse 488 (Alexa Fluor 488 goat anti-mouse, Invitrogen A11001); and rabbit 488 (Alexa Fluor 488 goat anti-rabbit, Invitrogen A11008). Sections were rinsed with PBS and nuclei labeled with 4,6-Diamidino-2-Phenylindole, Dihydrochloride (DAPI, dilactate, Invitrogen D3571). Antibody labeling was visualized, and representative images captured using a Leica DMI6000 fluorescent microscope (Leica Microsystems, Wetzlar, Germany) or a Nikon i90 microscope (Melville, New York, USA) equipped with fluorochrome appropriate band-pass filters16. Analysis of IHC images at approximately 100 µm retinal depth was performed by 2–3 individuals in a double-blinded manner. Fluorescence intensity of the opsins was measured using ImageJ to analyze mean gray values in each dose for both early and intermediate treatment groups at the 6 months post time point compared to untreated controls. The mean gray levels were between 0 and 85, with 0 indicating absence of fluorescence and 85 indicating maximum fluorescence intensity. The number of blue and green opsin-positive cells was also counted for the early and intermediate treatment groups at 6 months post-treatment.
Ethical approval
This study was carried out in strict accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals of the National Institute of Health, as well as the Association for Research in Vision and Ophthalmology (ARVO) Statement for the Use of Animals in Ophthalmic and Vision Research.
Data availability
All data used in this paper has been presented in the figures and supplementary files.
References
Daiger, S. P., Sullivan, L. S. & Bowne, S. J. Genes and mutations causing retinitis pigmentosa. Clin. Genet. 84, 132–141 (2013).
Ferrari, S. et al. Retinitis pigmentosa: Genes and disease mechanisms. Curr. Genomics 12, 238–249 (2011).
Hamel, C. Retinitis pigmentosa. Orphanet J. Rare Dis. 1, 40 (2006).
Pierrottet, C. O. et al. Syndromic and non-syndromic forms of retinitis pigmentosa: A comprehensive Italian clinical and molecular study reveals new mutations. Genet. Mol. Res. GMR 13, 8815–8833 (2014).
Mansergh, F. C. et al. Retinitis pigmentosa and progressive sensorineural hearing loss caused by a C12258A mutation in the mitochondrial MTTS2 gene. Am. J. Hum. Genet. 64, 971–985 (1999).
Daiger, S. P., Bowne, S. J. & Sullivan, L. S. Perspective on genes and mutations causing retinitis pigmentosa. Arch. Ophthalmol. Chic. Ill 1960(125), 151–158 (2007).
Bunker, C. H., Berson, E. L., Bromley, W. C., Hayes, R. P. & Roderick, T. H. Prevalence of retinitis pigmentosa in Maine. Am. J. Ophthalmol. 97, 357–365 (1984).
Bandah-Rozenfeld, D. et al. Homozygosity mapping reveals null mutations in FAM161A as a cause of autosomal-recessive retinitis pigmentosa. Am. J. Hum. Genet. 87, 382–391 (2010).
Grøndahl, J. Estimation of prognosis and prevalence of retinitis pigmentosa and Usher syndrome in Norway. Clin. Genet. 31, 255–264 (1987).
Haim, M. Epidemiology of retinitis pigmentosa in Denmark. Acta Ophthalmol. Scand. Suppl. https://doi.org/10.1046/j.1395-3907.2002.00001.x (2002).
Bhardwaj, A., Yadav, A., Yadav, M. & Tanwar, M. Genetic dissection of non-syndromic retinitis pigmentosa. Indian J. Ophthalmol. 70, 2355–2385 (2022).
Tsang, S. H. & Sharma, T. Autosomal dominant retinitis pigmentosa. Adv. Exp. Med. Biol. 1085, 69–77 (2018).
RetNet: Summaries. https://web.sph.uth.edu/RetNet/sum-dis.htm
Drag, S., Dotiwala, F. & Upadhyay, A. K. Gene therapy for retinal degenerative diseases: Progress, challenges, and future directions. Investig. Ophthalmol. Vis. Sci. 64, 39 (2023).
Sorrentino, F. S., Gallenga, C. E., Bonifazzi, C. & Perri, P. A challenge to the striking genotypic heterogeneity of retinitis pigmentosa: A better understanding of the pathophysiology using the newest genetic strategies. Eye 30, 1542–1548 (2016).
Li, S. et al. Nr2e3 is a genetic modifier that rescues retinal degeneration and promotes homeostasis in multiple models of retinitis pigmentosa. Gene Ther. 28, 223–241 (2021).
Haider, N. B. et al. The transcription factor Nr2e3 functions in retinal progenitors to suppress cone cell generation. Vis. Neurosci. 23, 917–929 (2006).
Haider, N. B., Naggert, J. K. & Nishina, P. M. Excess cone cell proliferation due to lack of a functional NR2E3 causes retinal dysplasia and degeneration in rd7/rd7 mice. Hum. Mol. Genet. 10, 1619–1626 (2001).
Coppieters, F. et al. Recurrent mutation in the first zinc finger of the orphan nuclear receptor NR2E3 causes autosomal dominant retinitis pigmentosa. Am. J. Hum. Genet. 81, 147–157 (2007).
Bernal, S. et al. Analysis of the involvement of the NR2E3 gene in autosomal recessive retinal dystrophies. Clin. Genet. 73, 360–366 (2008).
Hayashi, T. et al. Novel NR2E3 mutations (R104Q, R334G) associated with a mild form of enhanced S-cone syndrome demonstrate compound heterozygosity. Ophthalmology 112, 2115 (2005).
Escher, P. et al. Mutations in NR2E3 can cause dominant or recessive retinal degenerations in the same family. Hum. Mutat. 30, 342–351 (2009).
Haider, N. B. et al. Mutation of a nuclear receptor gene, NR2E3, causes enhanced S cone syndrome, a disorder of retinal cell fate. Nat. Genet. 24, 127–131 (2000).
Schorderet, D. F. & Escher, P. NR2E3 mutations in enhanced S-cone sensitivity syndrome (ESCS), Goldmann–Favre syndrome (GFS), clumped pigmentary retinal degeneration (CPRD), and retinitis pigmentosa (RP). Hum. Mutat. 30, 1475–1485 (2009).
Sharon, D., Sandberg, M. A., Caruso, R. C., Berson, E. L. & Dryja, T. P. Shared mutations in NR2E3 in enhanced S-cone syndrome, Goldmann–Favre syndrome, and many cases of clumped pigmentary retinal degeneration. Arch. Ophthalmol. Chic. Ill 1960(121), 1316–1323 (2003).
Gire, A. I. et al. The Gly56Arg mutation in NR2E3 accounts for 1–2% of autosomal dominant retinitis pigmentosa. Mol. Vis. 13, 1970–1975 (2007).
Nakamura, Y. et al. Enhanced S-cone syndrome in a Japanese family with a nonsense NR2E3 mutation (Q350X). Acta Ophthalmol. Scand. 82, 616–622 (2004).
Jacobson, S. G., Román, A. J., Román, M. I., Gass, J. D. & Parker, J. A. Relatively enhanced S cone function in the Goldmann–Favre syndrome. Am. J. Ophthalmol. 111, 446–453 (1991).
Tsang, S. H. & Sharma, T. Enhanced S-cone syndrome (Goldmann–Favre syndrome). Adv. Exp. Med. Biol. 1085, 153–156 (2018).
Ammar, M. J. et al. Enhanced S-cone syndrome: Visual function, cross-sectional imaging, and cellular structure with adaptive optics ophthalmoscopy. Retin. Cases Brief Rep. 15, 694–701 (2021).
Jacobson, S. G., Marmor, M. F., Kemp, C. M. & Knighton, R. W. SWS (blue) cone hypersensitivity in a newly identified retinal degeneration. Investig. Ophthalmol. Vis. Sci. 31, 827–838 (1990).
Milam, A. H. et al. The nuclear receptor NR2E3 plays a role in human retinal photoreceptor differentiation and degeneration. Proc. Natl. Acad. Sci. USA 99, 473–478 (2002).
Marmor, M. F., Jacobson, S. G., Foerster, M. H., Kellner, U. & Weleber, R. G. Diagnostic clinical findings of a new syndrome with night blindness, maculopathy, and enhanced S cone sensitivity. Am. J. Ophthalmol. 110, 124–134 (1990).
Jacobson, S. G. et al. Nuclear receptor NR2E3 gene mutations distort human retinal laminar architecture and cause an unusual degeneration. Hum. Mol. Genet. 13, 1893–1902 (2004).
Bonilha, V. L., Fishman, G. A., Rayborn, M. E. & Hollyfield, J. G. Retinal pathology of a patient with Goldmann–Favre syndrome. Ophthalmic Genet. 30, 172–180 (2009).
Ikäheimo, K., Tuppurainen, K. & Mäntyjärvi, M. Clinical features of Goldmann–Favre syndrome. Acta Ophthalmol. Scand. 77, 459–461 (1999).
Nishiguchi, K. M. et al. Recessive NRL mutations in patients with clumped pigmentary retinal degeneration and relative preservation of blue cone function. Proc. Natl. Acad. Sci. USA 101, 17819–17824 (2004).
Haider, N. B., Cruz, N. M., Allocca, M. & Yuan, J. Pathobiology of the outer retina: Genetic and nongenetic causes of disease. In Pathobiology of Human Disease (eds McManus, L. M. & Mitchell, R. N.) 2084–2114 (Academic Press, 2014).
Bandah, D., Merin, S., Ashhab, M., Banin, E. & Sharon, D. The spectrum of retinal diseases caused by NR2E3 mutations in Israeli and Palestinian patients. Arch. Ophthalmol. Chic. Ill 1960(127), 297–302 (2009).
Lotery, A. J. et al. Adeno-associated virus type 5: Transduction efficiency and cell-type specificity in the primate retina. Hum. Gene Ther. 14, 1663–1671 (2003).
Yang, G. S. et al. Virus-mediated transduction of murine retina with adeno-associated virus: Effects of viral capsid and genome size. J. Virol. 76, 7651–7660 (2002).
Pang, J. et al. Comparative analysis of in vivo and in vitro AAV vector transduction in the neonatal mouse retina: Effects of serotype and site of administration. Vis. Res. 48, 377–385 (2008).
Petit, L., Ma, S., Cheng, S.-Y., Gao, G. & Punzo, C. Rod outer segment development influences AAV-mediated photoreceptor transduction after subretinal injection. Hum. Gene Ther. 28, 464–481 (2017).
Long, B. R. et al. The impact of pre-existing immunity on the non-clinical pharmacodynamics of AAV5-based gene therapy. Mol. Ther. Methods Clin. Dev. 13, 440–452 (2019).
Wiley, L. A. et al. Assessment of adeno-associated virus serotype tropism in human retinal explants. Hum. Gene Ther. 29, 424–436 (2018).
Lee, S. H. et al. Transduction patterns of adeno-associated viral vectors in a laser-induced choroidal neovascularization mouse model. Mol. Ther. Methods Clin. Dev. 9, 90–98 (2018).
Garita-Hernandez, M. et al. AAV-mediated gene delivery to 3D retinal organoids derived from human induced pluripotent stem cells. Int. J. Mol. Sci. 21, 994 (2020).
Chen, J. & Nathans, J. Genetic ablation of cone photoreceptors eliminates retinal folds in the retinal degeneration 7 (rd7) mouse. Investig. Ophthalmol. Vis. Sci. 48, 2799–2805 (2007).
Chen, J., Rattner, A. & Nathans, J. Effects of L1 retrotransposon insertion on transcript processing, localization and accumulation: Lessons from the retinal degeneration 7 mouse and implications for the genomic ecology of L1 elements. Hum. Mol. Genet. 15, 2146–2156 (2006).
Akhmedov, N. B. et al. A deletion in a photoreceptor-specific nuclear receptor mRNA causes retinal degeneration in the rd7 mouse. Proc. Natl. Acad. Sci. USA 97, 5551–5556 (2000).
Rashid, K., Akhtar-Schaefer, I. & Langmann, T. Microglia in retinal degeneration. Front. Immunol. 10, 1975 (2019).
Guo, L., Choi, S., Bikkannavar, P. & Cordeiro, M. F. Microglia: Key players in retinal ageing and neurodegeneration. Front. Cell. Neurosci. 16, 804782 (2022).
Wu, J. et al. Activated microglia-induced neuroinflammatory cytokines lead to photoreceptor apoptosis in Aβ-injected mice. J. Mol. Med. Berl. Ger. 99, 713–728 (2021).
Yun, J.-H. Interleukin-1β induces pericyte apoptosis via the NF-κB pathway in diabetic retinopathy. Biochem. Biophys. Res. Commun. 546, 46–53 (2021).
Cheng, H., Khan, N. W., Roger, J. E. & Swaroop, A. Excess cones in the retinal degeneration rd7 mouse, caused by the loss of function of orphan nuclear receptor Nr2e3, originate from early-born photoreceptor precursors. Hum. Mol. Genet. 20, 4102–4115 (2011).
Auricchio, A. et al. Exchange of surface proteins impacts on viral vector cellular specificity and transduction characteristics: The retina as a model. Hum. Mol. Genet. 10, 3075–3081 (2001).
Haider, N. B. et al. Mapping of genetic modifiers of Nr2e3 rd7/rd7 that suppress retinal degeneration and restore blue cone cells to normal quantity. Mamm. Genome Off. J. Int. Mamm. Genome Soc. 19, 145–154 (2008).
Dvoriantchikova, G., Lypka, K. R. & Ivanov, D. The Potential role of epigenetic mechanisms in the development of retinitis pigmentosa and related photoreceptor dystrophies. Front. Genet. 13, 827274 (2022).
Fahim, A. T. et al. Allelic heterogeneity and genetic modifier loci contribute to clinical variation in males with X-linked retinitis pigmentosa due to RPGR mutations. PLoS One 6, e23021 (2011).
Berson, E. L., Rosner, B., Sandberg, M. A., Weigel-DiFranco, C. & Willett, W. C. Omega-3 intake and visual acuity in patients with retinitis pigmentosa on vitamin A. Arch. Ophthalmol. 130, 707–711 (2012).
Olivares, A. M. et al. Multimodal regulation orchestrates normal and complex disease states in the retina. Sci. Rep. 7, 690 (2017).
Corbo, J. C. & Cepko, C. L. A hybrid photoreceptor expressing both rod and cone genes in a mouse model of enhanced S-cone syndrome. PLoS Genet. 1, e11 (2005).
Craft, C. M., Huang, J., Possin, D. E. & Hendrickson, A. Primate short-wavelength cones share molecular markers with rods. Adv. Exp. Med. Biol. 801, 49–56 (2014).
Haider, N. B. et al. Nr2e3-directed transcriptional regulation of genes involved in photoreceptor development and cell-type specific phototransduction. Exp. Eye Res. 89, 365–372 (2009).
Peng, G.-H., Ahmad, O., Ahmad, F., Liu, J. & Chen, S. The photoreceptor-specific nuclear receptor Nr2e3 interacts with Crx and exerts opposing effects on the transcription of rod versus cone genes. Hum. Mol. Genet. 14, 747–764 (2005).
Liu, K., Zou, C. & Qin, B. The association between nuclear receptors and ocular diseases. Oncotarget 8, 27603–27615 (2017).
Yen, P. M. Classical nuclear hormone receptor activity as a mediator of complex biological responses: A look at health and disease. Best Pract. Res. Clin. Endocrinol. Metab. 29, 517–528 (2015).
Olivares, A. M., Moreno-Ramos, O. A. & Haider, N. B. Role of nuclear receptors in central nervous system development and associated diseases. J. Exp. Neurosci. 9, 93–121 (2015).
Acknowledgements
We are very grateful to Dr. David Van Vector and Hansine Heggeness for providing lab space, reagents, and access to a microscope. We thank Dr. Petr Baranov, Dr. Dong Feng Chen and Dr. Anton Lennikov for their input. We thank Maiya Whalen, Andrew Luo and Steven Portillo for technical assistance. We thank the Gene Transfer Vector Core and the SERI-MEE Morphology, Microscopy, and Animal Facilities for their services (NIH: National Eye Institute, Grant # P30EY003790).
Funding
This work was supported by the following funding agencies: Ocugen INC (NBH), and American Macular Degeneration Foundation (NBH).
Author information
Authors and Affiliations
Contributions
Conceived and designed the study: NBH. Intellectual discussions: MMD, PS, AKU. Conducted the experiments: SMM, MA, ZL, NN. Analyzed the data: NBH, SMM, MA, ZL, NN, KN. Wrote and edited the manuscript: SMM, NBH.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
McNamee, S.M., Akula, M., Love, Z. et al. Evaluating therapeutic potential of NR2E3 doses in the rd7 mouse model of retinal degeneration. Sci Rep 14, 16490 (2024). https://doi.org/10.1038/s41598-024-67095-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-67095-6
- Springer Nature Limited