Abstract
The gastric epithelium is often exposed to injurious elements and failure of appropriate healing predisposes to ulcers, hemorrhage, and ultimately cancer. We examined the gastric function of CD36, a protein linked to disease and homeostasis. We used the tamoxifen model of gastric injury in mice null for Cd36 (Cd36−/−), with Cd36 deletion in parietal cells (PC-Cd36−/−) or in endothelial cells (EC-Cd36−/−). CD36 expresses on corpus ECs, on PC basolateral membranes, and in gastrin and ghrelin cells. Stomachs of Cd36−/− mice have altered gland organization and secretion, more fibronectin, and inflammation. Tissue respiration and mitochondrial efficiency are reduced. Phospholipids increased and triglycerides decreased. Mucosal repair after injury is impaired in Cd36−/− and EC-Cd36−/−, not in PC-Cd36−/− mice, and is due to defect of progenitor differentiation to PCs, not of progenitor proliferation or mature PC dysfunction. Relevance to humans is explored in the Vanderbilt BioVu using PrediXcan that links genetically-determined gene expression to clinical phenotypes, which associates low CD36 mRNA with gastritis, gastric ulcer, and gastro-intestinal hemorrhage. A CD36 variant predicted to disrupt an enhancer site associates (p < 10−17) to death from gastro-intestinal hemorrhage in the UK Biobank. The findings support role of CD36 in gastric tissue repair, and its deletion associated with chronic diseases that can predispose to malignancy.
Similar content being viewed by others

Introduction
In addition to assisting the gut in nutrient absorption through the secretion of acid and digestive enzymes, the stomach influences metabolic homeostasis through releasing hormones, such as ghrelin and leptin that have systemic effects. Gastric functions are regulated by food intake, the vagus nerve, and in an autocrine manner1. Gastric ghrelin, released during fasting, acts in the brain to increase food intake and in adipose tissue to promote energy storage2,3 in addition to having protective cardiovascular actions4. Gastric leptin, unlike adipose leptin which is constitutive, responds to feeding and vagal input to regulate short-term energy metabolism5,6. Leptin also has positive effects on epithelial cell proliferation7 and small intestinal growth8,9. Other secretions by the stomach include gastrin and somatostatin, with opposite actions on gastric acid secretion and with numerous effects on organs beyond the stomach10, and gastric intrinsic factor (GIF) essential for intestinal vitamin B12 absorption11.
As a port of entry for food, drugs, and pathogens, the gastric mucosa is continuously subjected to injury from chemicals and microbes. The organ’s ability to recover from insults depends on the renewal of its epithelial cells. Superficial injury of the gastric mucosa, such as occurs after ethanol, can be repaired rapidly while deeper mucosal injury consequent to aspirin or non-steroidal agents (NSAIDS) or H. pylori infection heals more slowly12,13. Appropriate repair is required to prevent gastritis, ulcers, hemorrhage, and the development of metaplasia14. Although cellular metabolism influences cell fate and function and is dysregulated in disease15,16,17, its role in maintaining the gastric epithelium is unclear. In particular, fatty acid (FA) uptake and FA oxidation have been shown important for tissue maintenance and repair, most notably by keeping a competent niche of stem cells. Although FA oxidation does not acutely fuel proliferation of stem cells, it is critical for maintaining the stem cells’ long-term ability to differentiate18,19.
The scavenger receptor CD36 was reported to be abundant in stomach tissue20 and its mRNA identified a decade ago in a microarray of magnetic bead sorted parietal cells21. CD36 facilitates FA uptake and FA oxidation so we investigated if gastric CD36-mediated FA metabolism is important for the function and repair of the gastric mucosa.
In addition to facilitating FA uptake, CD36 mediates signal transduction important in metabolic regulation22 and tissue homeostasis23,24. In the small intestine, CD36 is important for optimal secretion of chylomicrons25, the release of regulatory gut peptides26 and the protection of barrier integrity24. In the present study, we document the influence of CD36 on stomach biology, function, and recovery from injury. The impact of global versus cell-targeted Cd36 deletion pinpoints to the critical role of tissue lipid metabolism in epithelial renewal. We also identify genetic associations in two large patient databases between the CD36 expression and gastric disease.
Results
Cd36 deletion alters gastric gland morphology, gastric secretions, and increases matrix accumulation
The CD36 protein level is robust in the mouse stomach, (Supplementary Fig. 1a). Among the forestomach, corpus, and antrum, CD36 is most abundant in the corpus (Supplementary Fig. 1b). Unlike in the small intestine27, the CD36 level is unchanged by fasting and refeeding (Supplementary Fig. 1c).
In the corpus of wildtype (WT) mice, gastric glands line up alongside vessels that run from the lumen to the base of the epithelium. In Cd36−/− mice, there is frequent misalignment with inconsistency in the relative length of neck and base zones (Fig. 1a). CD36 is most abundant in endothelial cells, ECs (Fig. 1b). CD36 is also present exclusively on parietal cells among gastric epithelial cells as documented by laser captured microdissected cells and using mice with lineage-specific GFP expression in parietal cells28,29. Here we show that CD36 localizes to the parietal cell (PC) basolateral side adjacent to ECs and is excluded from the luminal side, identified by apical membrane-associated ezrin (Fig. 1c). CD36 localization on PCs contrasts with its apical lumen-facing localization in small intestinal enterocytes26,30 and suggests that it does not function in nutrient absorption from the gastric lumen. CD36 is present in ghrelin and gastrin cells (Fig. 1d-e) but absent from chief (GIF staining), enteroendocrine (chromogranin A), foveolar/pit, mucous neck, and tuft (Doublecortin like kinase-1, DCLK1) cells (Supplementary Fig. 1d–f). In summary, in the stomach CD36 is expressed in parietal, endothelial and some enteroendocrine cells. The higher CD36 expression in the corpus as compared to the antrum can be related to the higher vascularization of the corpus and the lack of parietal cells in the antrum. The expression on enteroendocrine cells (gastrin and ghrelin) does not contribute significantly to total CD36 expression levels since these cells are a small percent (1–2%) of total cells in the mucosa.
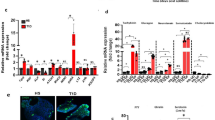
a Representative histology and immunohistochemistry of a stomach from a wildtype (WT) mouse (left) and a Cd36−/− mouse (right) showing the altered organization of acid-producing parietal cells (PC) around blood vessels in gastric glands (blue asterisks). b CD36 expression in the corpus is most abundant on endothelial cells and is also detected in PCs. c In PCs, CD36 (red) is at the basolateral membrane (dotted yellow line) and is excluded from the apical membrane marked by ezrin (magenta) and in contact with the lumen (blue dotted line). d, e Immunostaining for ghrelin and gastrin (right insets: magnification of cell markers colocalized with CD36). Scale bar: 50 µm, except for c and inserts in d, e (10 µm). b–e are stomachs from WT mice. Scale bar: 50 µm. f–i mRNA for hormones in fasted or 4 h refed mice. All mRNA adjusted to 36b4. j Plasma gastrin and k plasma leptin in fasted or 4 h refed mice. SST somatostatin. Significance was calculated using a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons. *P < 0.05, **P < 0.01, ***P < 0.001. Data are means ± SEM, f–i: n = 5, j n = 7, k n = 8.
Cd36 deletion did not alter gastric mRNA levels of genes specific to PCs; ATP4B, VEGFB, neck cells; Tff1, pit cells; mucin (Muc5AC) or the enteroendocrine cell marker chromogranin A (ChA) (Supplementary Fig. 1g). The mRNA for gastrin was higher, those for somatostatin and ghrelin lower (Fig. 1f–h). The mRNA for leptin was almost completely (94%) suppressed (Fig. 1i). Plasma gastrin levels were higher at 4 h refeeding (Fig. 1j) in Cd36−/− mice in parallel to tissue mRNA and in line with the stomach being the main source of gastrin.
In contrast to the constitutive and slow leptin secretion by adipose tissue5,31, gastric leptin is released by chief cells32,33 in a rapidly regulated secretion pathway sensitive to vagal input and raises circulating leptin after hormone stimulation (pentagastrin and cholecystokinin) or food intake6,32,33,34. Plasma leptin in fasted Cd36−/− and WT mice did not differ, but leptin increase at 4 h after refeeding was blunted in Cd36−/− mice (Fig. 1k). We examined if this reflects the absence of the established role of CD36 in mediating orosensory fatty acid perception by mouth taste buds, transmitted via the gustatory nerve. This perception is integral to vagal regulation of early cephalic responses to food intake35,36,37. Cephalic responses were determined at 15 min after an oral fat meal in fasted WT and Cd36−/− mice. Leptin levels increased in WT mice and the increase was suppressed in Cd36−/− mice (Fig. 2a). Nongastric responses such as plasma insulin (Fig. 2b) and pancreatic polypeptide (Fig. 2c) were almost absent in Cd36−/− mice. Stomach acetylcholine was reduced in Cd36−/− mice (Fig. 2d). These data indicated that impaired orosensory FA sensing reduces vagal input after food intake and consequently the gastric secretion of leptin.
a–c Impaired response of plasma leptin, insulin, and pancreatic polypeptide in fasted mice and 15 min after an oral high fat meal. d Stomach acetylcholine levels in 4 h refed mice. e,f Gastric secretions at 1 h after pylorus ligation in 18 h fasted mice given i.p. saline (Control), carbachol (CCh, 60 µg/kg) or histamine (H, 10 mg/kg). e Gastric juice pH. f Immunoblots of gastric juice; quantification of gastric intrinsic factor (GIF)/total protein in juice showing reduced GIF output in Cd36−/− mice given carbachol. g Chief cells markers by qPCR and immunostaining (green) in corpus of wildtype (WT) and Cd36−/− mice, scale: 50 µm. h mRNA of muscarinic receptor 1 (M1r) in the corpus of WT and Cd36−/− mice. Significance was calculated using a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons or a two-sided unpaired t test (d and h). *P < 0.05, **P < 0.01. a–c n = 4–5 per condition/group; d: n = 7–12; e,f n = 3–4; g,h n = 5.
Acid secretion by PCs is upregulated by gastrin and acetylcholine and inhibited by somatostatin (SST)38. Gastrin stimulates ECL cell release of the secretagogue histamine and potentiates cholinergic action in PCs. Surprisingly, gastric acid secretion, examined using pylorus-ligation before and after the cholinomimetic carbachol or histamine, was similar for WT and Cd36−/− mice (Fig. 2e). However, carbachol-induced secretion of gastric intrinsic factor (GIF) by chief cells was reduced in Cd36−/− stomachs (Fig. 2f) although GIF expression was unchanged (Fig. 2g). Expression of M1 muscarinic receptors, primarily found in chief cells39 was higher (Fig. 2h), possibly a compensatory effect to the low GIF output, while expression of M3 and M4, involved in PC acid secretion40 was unchanged. Thus, Cd36−/− stomachs do not display defective carbachol stimulation of acid secretion while carbachol stimulated GIF release is reduced, suggesting selective muscarinic receptor impairment.
Corpus morphology by transmission electron microscopy (TEM) showed in Cd36−/− tissue altered interface between PCs and endothelial cells (Fig. 3a, blue asterisks and white arrows), with Cd36−/− PCs harboring abundant mitochondria within the normally mitochondria-free region of interface between the PCs and ECs. This area normally accumulates VEGFB, suggesting it is critical for PC communication with endothelial cells and exchange of metabolites with the blood29. Extracellular matrix (ECM) remodeling was evident under steady state conditions in stomachs from nonfasted Cd36−/− mice; specifically higher mRNA for fibronectin (Fig. 3b) and fibronectin deposition around vessels and in submucosa (Fig. 3c). Other ECM markers, including laminin and collagen 1α did not change (Fig. 3b). Inflammation markers assessed during fasting and refeeding showed higher expression in Cd36−/− tissue; IL6, the chemokine MIP-2, which regulates leukocyte recruitment, and the neutrophil marker S100A8 were increased while anti-inflammatory IL10 trended lower (Fig. 3d). These data suggest compromised gastric tissue in Cd36−/− mice.
a Transmission electron microscopy (TEM) of parietal cells in the Cd36−/− corpus show a lack of mitochondria-free area at the basolateral side (blue asterisks) and ECM deposits between the PC membrane and blood vessels (white arrows). Scale bars: 6 µm (top) and 1 µm (bottom) panels. b mRNA of ECM proteins fibronectin, laminin and collagen1α in nonfasted mice. c Immunostaining of fibronectin (green) in corpus of WT and Cd36−/− mice. Scale bar: 50 µm. d mRNA of inflammation and neutrophil markers. Significance was calculated using a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons. *P < 0.05, **P < 0.01, ***P < 0.001. Data are means ± SEM. b n = 7, d n = 5.
Epithelial renewal after injury is impaired in stomachs from Cd36 -/- mice
The gastric epithelium can experience injury from pathogens, alcohol or drugs, and PC renewal is critical to the tissue’s repair ability. The presence of ECM remodeling and inflammation in the Cd36−/− stomach prompted us to examine its response to stress. We used the acute injury model of high-dose tamoxifen (TAM), which causes PC-targeted, estrogen-independent toxicity that kills nearly all PCs41,42. As this is followed by rapid de novo PC renewal, progenitor proliferation and differentiation into gastric units can be evaluated. Lineage commitment can also be assessed from measuring the fraction of proliferating chief cells expressing neck cell markers, such as Griffonia Simplicifolia lectin II (GSII), referred to as SPEM cells43. Mice were TAM injected for 3 days and gastric recovery evaluated 5 days later. As expected41,42, TAM induced PC atrophy in WT and Cd36−/− mice to the same extent and increased cell proliferation throughout the gastric glands in both groups (Supplementary Fig. 2a–c). However, gland recovery differed between genotypes, while at day 5 post-TAM, proliferation (Fig. 4a, d) and PC atrophy (Fig. 4b, e) were largely reversed in WT mice, in Cd36−/− mice although proliferation was reversed, PC renewal was 41% lower than WT mice. This indicated suboptimal progenitor differentiation to PC, and the new glands were abnormally elongated (Fig. 4f). Consistent with a differentiation defect, the fraction of chief cells that had undergone palingenosis to the metaplastic, proliferative SPEM lineage (SPEM cells co-express neck and chief cell markers; GSII+/GIF+) was 60% higher in the Cd36−/− relative to the WT corpus (Fig. 4g). The lower PC renewal and increase in SPEM cells indicate that defects in progenitor differentiation to PCs and in lineage commitment drive the impairment of mucosal renewal.
a–c Representative histology and immunohistochemistry of wildtype (WT) and Cd36−/− mice that were either untreated (control), or injected with TAM for 3 days followed by 5 days of recovery (TAM + D5); a proliferation marker ki67; b vascular endothelial growth factor B (VEGFB), red; ezrin, green; c GIF, green; GSII, red. Scale bar: 50 µm. Quantification of d ki67+ cells and e parietal cells per gastric unit, f gland length, and g GIF/GSII+ cells per gastric unit (yellow). Significance was calculated using a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons. *P < 0.05, **P < 0.01. Data are means ± SEM, n = 3 mice/group.
Cd36 deletion reduces stomach FA uptake and mucosal respiration
FA oxidation is particularly critical for tissue stem cells18,44 and reduced FA oxidation impairs stem cell functionality and the ability for optimal differentiation45. We examined the effect of Cd36 deletion on gastric FA metabolism. Deletion of Cd36 reduces FA uptake in heart, skeletal muscle, and fat tissue but reduction is not observed in other tissues such as liver or kidney46. To our knowledge, uptake of long-chain FA by the stomach has not been examined whether in the presence or absence of CD36. Mice intravenously injected with [3H]oleic showed robust oleic acid uptake by the corpus and uptake was significantly reduced in Cd36−/− mice (Fig. 5a). We next determined if the reduced uptake alters tissue oxygen consumption by corpus mucosa from WT and Cd36−/− mice. The Cd36−/− mucosa consumed 26% less oxygen in the oxidative phosphorylative state (OxPhos C-I and C-II) and had lower maximal respiratory flux (ETS) (Fig. 5b). Mitochondrial coupling efficiency (of oxidation and ATP synthesis, RCR) trended lower in Cd36−/− compared to WT mucosa (P = 0.07, Fig. 5c). Mitochondrial FA oxidation was determined by mass spectrometry of oxidation intermediates. The Cd36−/− stomachs had lower levels of short-chain acylcarnitines but accumulated long-chain acylcarnitines, a pattern indicative of inefficient mitochondrial FA oxidation47,48 (Fig. 5d). In addition, cardiolipin, an essential constituent of the inner mitochondrial membrane, increased in refed Cd36−/− stomachs and had higher polyunsaturated FA content (Fig. 5e, f), a remodeling similar to that described in aging and early stages of diabetes49,50. These functional abnormalities associated with morphological changes in mitochondria (Fig. 5g, h), which were more circular with a reduced aspect ratio (major/minor axis, Fig. 5h). Together these studies show that the corpus relies on circulating FA, and chronically reducing FA supply reduces mitochondrial efficiency, and diminishes tissue respiration and mitochondrial FA oxidation, which impairs PC progenitor ability for optimal differentiation to PCs.
a Tissue uptake of oleic acid in wildtype (WT) and Cd36−/− mice. Four-month-old mice 16 h fasted mice, were given a retro-orbital injection of [3H]oleic acid and tissues collected 5 min later for measuring radioactivity. b High-resolution respirometry (Oxygraph-2k) of permeabilized corpus mucosa from WT and Cd36−/− mice. Leak: plus malate (1 mM), glutamate (10 mM) and pyruvate (5 mM). OxPHOS: Oxygen consumption, plus ADP (5 mM) and succinate (10 mM). ETS: Maximum flux after FCCP uncoupling. c Ratio of OxPHOS/leak in WT and Cd36−/− mucosa showing trend for lower coupling efficiency. d Cd36−/− stomachs have lower levels of short-chain acylcarnitines but accumulate long-chain acylcarnitines. e, f cardiolipin (CL) enrichment with ω6 PUFA. g transmission electron microscopy (TEM) showing altered morphology of PC mitochondria (arrow) in Cd36−/− mice, scale bar: 2 µm. h Mitochondrial circularity and aspect ratio (major/minor axis). Significance was calculated using a two-sided unpaired t test or a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons (e, f, and h). *P < 0.05, *P < 0.01, ***P < 0.001, ****P < 0.0001. Data are means + SEM. a n = 4–5; b–c n = 4; d–f n = 7–12; h n = 600 mitochondria from 9 PCs/genotype.
The Cd36 -/- stomach is depleted of TAG and has higher phospholipids
Untargeted lipidomic analyses showed that stomachs from fasted Cd36−/− mice had depleted triglycerides (TAG) (Fig. 6a) whether diet-derived or de novo synthesized (Supplementary Fig. 3a) while phospholipids are increased. Refeeding increased TAG and diacylglycerols (DAG) in WT stomachs, but most TAGs remained reduced in Cd36−/− stomachs (Fig. 6a, b) while phosphatidylcholine (PC), phosphatidylethanolamine (PE) (Fig. 6a, c), and phosphatidylglycerol (PG) increased (Fig. 6a). Increase of the percent phospholipid has been reported in chronic atrophic gastritis and gastric ulcers51. In addition, there was the remodeling of PC and PE polyunsaturated FA (PUFA) with higher percent arachidonic acid (ω6 20:4) (Fig. 6d) and ratio of 20:4 to ω3 FA (20:5, 22:5 and 22:6). Consistent with lack of TAG/DAG response to refeeding, Cd36−/− mice had lower mRNA of a key TAG synthesis enzyme GPAT4 and failed to increase mRNA levels of AGPAT1 after refeeding, while adipose triglyceride lipase (ATGL), the key to FA mobilization, increased during fasting in line with depletion of TAG stores (Fig. 6e, f). Expression of glycolytic enzymes was unchanged, but pyruvic and lactic acids (Supplementary Fig. 3b) and Krebs cycle fumarate and malate (Supplementary Fig. 3c) were reduced. Thus, CD36 deletion remodels gastric tissue lipids as TAG are depleted and phospholipids increase, the latter change reminiscent of trends reported in gastritis and ulcers51.
a Heat map of top 60 metabolites/lipids in fasted and re-fed wildtype (WT) and Cd36−/− stomach. b The sum of identified diacylglycerol (DAG) and triacyglycerol (TAG) species was reduced in Cd36−/− stomachs. c Cd36 deficient stomachs accumulate more phospholipids with d higher % of 20:4. e Cd36−/− mice have lower mRNA levels of TAG synthesis enzyme glycerol-3-phosphate acyltransferase 4 (GPAT4) but increased levels of the TAG lipolytic enzyme adipose triglyceride lipase (ATGL). f Schematic summary of key steps in TAG synthesis with intermediates that serve as precursors of other lipid species, such as phospholipids (PL). CL cardiolipin, FA fatty acids, MAG monoacylglycerol, PC phosphatidylcholine, PE phosphatidylethanolamine, PG phosphatidylglycerol, PI, phosphatidylinositol, PS, phosphatidylserine, PUFA, polyunsaturated FA. Significance was calculated using a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons. *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001. Data are means ± SEM, n = 7–12 mice/group for a–d, and n = 5 for e.
Deletion of Cd36 in parietal cells does not alter the response to injury
The impaired recovery from injury in Cd36−/− stomachs reflected dysfunction of PC progenitor differentiation. We examined if CD36 absence in mature PCs can drive the defect in epithelial renewal. We generated a mouse model with PC-specific Cd36 deletion (PC-Cd36−/−) (Supplementary Fig. 4a). The Cd36−/− PCs, like PCs of Cd36−/− mice, showed mitochondrial migration toward adjacent capillaries but no alterations in the plasma membrane or in the appearance of mitochondria (Supplementary Fig. 4b, c). The corpus did not show altered expression of markers for PCs, gastrin, or genes related to ECM remodeling or inflammation (Supplementary Fig. 4d, e). Unlike in Cd36−/− mice, oleate uptake by the corpus was unchanged in PC-Cd36−/− mice (Supplementary Fig. 4f). The PC-Cd36−/− stomachs recovered from TAM injury like those of floxed controls (Supplementary Fig. 5a–d). These data show that while global Cd36 deficiency results in dysfunctional progenitors and reduced PC renewal, deletion of Cd36 in mature PC is not, by itself, sufficient to cause the corpus abnormalities and delayed injury recovery seen in Cd36−/− stomachs.
Cd36 deletion in endothelial cells reduces stomach FA uptake and recapitulates major gastric abnormalities of Cd36 -/- mice
Recent findings documented a primary role of endothelial cell CD36 in FA uptake by the heart, muscle, and brown adipose tissue46. As in these tissues, CD36 in the stomach is most robustly expressed on ECs in the corpus. We examined if EC-Cd36−/− mice can recapitulate the morphologic and metabolic alterations and the delayed PC recovery observed in Cd36−/− stomachs. Similar to Cd36−/− mice and unlike PC-Cd36−/− mice (Supplementary Fig. 4f), the EC-Cd36−/− mice (Fig. 7b) had reduced corpus uptake of injected [3H]oleate. The EC-Cd36−/− stomachs displayed many of the abnormalities seen in Cd36−/− mice; mitochondrial migration towards capillaries in PCs, remodeling of mitochondrial cardiolipin with enrichment in ω6 PUFA, less elongated mitochondria with a reduced aspect ratio (Fig. 7c–e) and increases in MCP1 and fibronectin (Fig. 7f, g).
a Gastric sections from floxed controls (left panels) and EC-Cd36-/- mice (right panels) showing absence of CD36 expression in the gastric endothelium and CD36 expression in parietal cells (PCs) (white arrows, bottom right). Scale bars: 50 µm (top) and 20 µm (bottom) panels. b Corpus uptake of oleic acid is reduced in EC-Cd36−/− mice. 16 h fasted 4-month-old mice were given a retro-orbital injection of [3H]oleic acid and tissues collected for measuring radioactivity 5 min later. c Sum of cardiolipin species enriched with ω6 PUFA d Transmission EM showing EC-Cd36−/− PCs lack the mitochondria (“M”)-free area near the plasma membrane bordering capillaries (right panel). Scale bar: 2 µm. e Quantification of mitochondrial circularity and aspect ratio (major/minor axis). f mRNA expression of gastric hormones, fibronectin, and inflammatory markers in corpus of EC- Cd36−/− mice. g Fibronectin staining (green) in corpus of control and EC-Cd36−/− mice, scale bar: 50 µm. Significance was calculated using a two-sided unpaired t test or a two-way ANOVA followed by post hoc tests by Sidak multiple comparisons (c). *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001. Data are means + SEM. b n = 6; c n = 8–9; e n = 1500 mitochondria from 11 PCs/genotype; f n = 6.
Untargeted metabolomic-lipidomic analyses revealed that EC-Cd36−/− stomachs (Supplementary Fig. 6a–b) like Cd36−/− stomachs had reduced diet-derived TAG although de novo TAG species increased, reflecting more glucose utilization for lipogenesis, likely due to CD36 presence in PCs (Fig. 7a). As in Cd36−/− mice, PC and PE had more percent 20:4 and higher 20:4 to ω3-PUFA ratios (Supplementary Fig. 6d). However, unlike the Cd36−/− mice which survived the TAM protocol, the EC-Cd36−/− mice in two separate experiments died during the recovery phase. The reason for the mortality is unclear and suggests unresolved inflammation from the combination of gastric damage after TAM with damage from Cd36 deletion in endothelial cells.
Low CD36 expression associates with stomach disorders in humans
The current findings suggest that CD36 deficiency impairs gastric recovery from injury that would predispose to pathology, so we explored their potential human relevance. PrediXcan analysis, which estimates the genetic component of gene expression using models trained with reference transcriptome data (v8) from the Genotype-Tissue Expression (GTEx) Consortium52,53, was applied to Vanderbilt University’s BioVU genomic resource where electronic health records (EHR) are tied to whole-genome genetic information54. We identified significant associations between genetically reduced CD36 expression and increased incidence of gastric ulcer, gastritis, duodenitis, and nonspecific hemorrhage of the gastrointestinal tract (Table 1). These findings support the functional data in mice and further suggest that CD36 is also likely important for the maintenance of the gut epithelium. In line with this, exploration of the UK Biobank, another large-scale EHR database that combines in-depth genetic and health information from half a million UK participants55 identified a CD36 SNP rs144921258 that strongly associates (p = 7.9e-17) with gastrointestinal hemorrhage as the underlying primary cause of death (Fig. 8a). The SNP’s top association is this phenotype across 1403 binary phenotypes tested. The SNP occurs primarily in individuals of European ancestry with 0.15 % minor allele frequency. It lies in intron 1 close to the major 1B promoter of CD36 (Fig. 8b) where it is predicted to disrupt an enhancer element based on H3K4me1 CHiP-Seq data from Roadmap Epigenomics Consortium56. The gene area where the SNP localizes is rich in epigenetic signatures (H3K4me1, H3K4me2, H3K4me3, H3K27ac) and methylation sites57. Fig. 8b shows the position of the SNP relative to those previously associated to methylation sites (CpG) and to reductions of CD36 expression and lipid handling57.
a Genomic coordinates along chromosome 7q (x-axis), with negative logarithm of p-values (y-axis) for SNP association with gastrointestinal hemorrhage p = 7.9-17. Location of rs144921258 in CD36 on chr7q is indicated by a diamond. The schematic of the CD36 gene below the plot also depicts the position of GNAT3, which overlaps a distal promoter of CD36. b Position of rs144921258 relative to the abundant proximal CD36 promoter 1B, (shown with its long 3’ untranslated region) and to SNPs previously associated with methylation at CpG sites with impact on CD36 expression and lipid handling. Red CpGs: SNP-associated methylation sites that impact CD36 expression. Purple SNPs: SNPs associated with both lipid levels and low CD36 expression. See also Table 1 and Results.
Discussion
Little attention has been paid to understanding the metabolism of the gastric mucosa although it could shed light on the etiology of common gastric diseases. In this study, metabolic and functional findings in three mice models of Cd36 deficiency provide strong support for the critical role of CD36 in maintaining optimal gastric tissue function and the ability for self-renewal postinjury (Fig. 9). The major contributions of the work are the following. First, we show that Cd36 deletion impairs gastric function, metabolism, and mucosal renewal after injury, through reducing endothelial cell delivery of fatty acids to the corpus and not by damaging parietal cell function. Second, as with other stem cell populations, the long-term defect in FA uptake and oxidation was found to result in less competent progenitor cells that are not amenable to full differentiation into parietal cells, impeding tissue recovery from injury. Finally, the defective release of leptin by the CD36 deficient stomach is an additional potential contributor to the impaired gastric recovery. The clinical impact of our work is highlighted by the finding that the defect of gastric recovery in low CD36 expression might be one underlying mechanism in the etiology of ulcer, gastritis, and gastrointestinal hemorrhage.
CD36 is abundant in corpus endothelial cells (EC) and expressed in parietal cells (PC). It is not detected in chief cells (CC), but its deficiency through vagal input and likely muscarinic receptor 1, suppresses CC release of leptin and gastric intrinsic factor (GIF), respectively. GIF is necessary for ileal vitamin B12 absorption. CD36 deletion reduces endothelial delivery of fatty acids to the corpus, tissue energy stores and mitochondrial FA oxidation, critical for stem cell functionality. Impaired renewal of the CD36-/- gastric epithelium reflects defective PC progenitor differentiation to PCs and not progenitor proliferation or dysfunction of mature PCs. Low gastric leptin secretion could further impair tissue healing. The reduced tissue ability for adequate repair would contribute to the etiology of gastric disease, as supported by data from two biomedical databases (see Fig. 8 and Table 1).
CD36 deficiency altered stomach release of gastrin, GIF, and leptin. In particular suppressed release of GIF which is required for intestinal B12 absorption, chronically could cause B12 deficiency that is unresponsive to oral B12 supplementation. GIF binds B12 in the duodenum and transports it to the ileum where it is absorbed. B12 deficiency causes neuronal demyelination, cognitive impairment, and macrocytic anemia11,58.
The gastrin increase in CD36 deficiency did not correlate with hypochlorhydria and was probably due to the reduced somatostatin, which inhibits gastrin gene expression and its release59. The high gastrin in Cd36−/− stomachs likely sustains acid secretion despite the diminished vagal input60.
Leptin and ghrelin play a significant role in energy balance, having opposite functions in regulation of hunger and satiety. In the stomach, food intake inhibits ghrelin secretion, while it increases that of leptin2,3,6,31. In the present study, CD36 deficiency decreased stomach mRNA levels of both hormones. Leptin secretion usually measured in the circulation reflects adipose tissue leptin, as the contribution of stomach leptin release is only significant early after a meal. Regulation of leptin secretion by food intake differs between the adipose and stomach tissues, with slow versus rapid responses of adipose and stomach leptin, respectively5,31. Thus, immediately after feeding the change in circulating leptin reflects gastric leptin secretion. In CD36 deficiency the marked reduction in leptin secretion consequent to low vagal input could have contributed to the defect in mucosal recovery from injury in the stomach since gastric leptin which reaches the intestine was shown important for intestinal and gastric maintenance9,61,62.
Uptake of circulating FAs by corpus endothelial cells was found necessary to maintain tissue energy stores and FA oxidation. CD36 upregulates FA oxidation in vivo63,64 and in vitro through activation of AMPK and PPAR delta22,65. FA oxidation is particularly critical for tissue stem cells18,44 as reduced FA oxidation impairs stem cell functionality45 and ability for optimal differentiation15. In the tamoxifen gastric injury model, we document that CD36 deletion suppresses the conversion of PC progenitors into PCs despite similar progenitor proliferation. Moreover, deeper in the gland, the number of GIF/GSII positive SPEM cells generated by palingenosis from chief cells66 is increased, and the new glands are often abnormally elongated. Thus, in addition to PC progenitors, both isthmal/neck and chief cell progenitor zones are affected by the loss of CD36.
Unlike Cd36 deletion in ECs, its deletion in parietal cells did not reduce corpus FA uptake and did not reproduce the above abnormalities. Thus, the endothelium is a gatekeeper in gastric tissue FA uptake, and CD36 in PCs like CD36 in muscle cells, alone is not sufficient to cause tissue-wide abnormalities46. The data are also consistent with the primary role of dysfunctional progenitor differentiation rather than of dysfunctional PCs in the defect in gastric renewal.
The reduced FA uptake in the corpus increased phospholipids and phosphatidylglycerol (PG), similar to findings in gastric and duodenal specimens from patients with gastritis and ulcer51. The increase and remodeling of phospholipids with more percent arachidonic acid might be less protective of the gastric mucosa in addition to potentially yielding more arachidonic acid derived proinflammatory eicosanoids67. In contrast, higher PG, an inflammation-responsive lipid, reduces activation of toll-like receptors68.
The association of low CD36 mRNA with gastric ulcer, gastritis, duodenitis, and gastrointestinal hemorrhage in the BioVu database suggests CD36 is critical for human gastric homeostasis. The PrediXcan approach, which examines the genetic component of gene expression using models trained with reference transcriptome data, increases the likelihood that associations observed between the expression of a gene and phenotypes are causal52,53. This interpretation is further buttressed by the identification of a previously unstudied CD36 SNP that strongly associates with death from gastrointestinal hemorrhage in the UK Biobank, providing additional support for relevance of the CD36 gene to gastrointestinal pathology. The SNP would disrupt the site directing a methylated histone H3K4me1 that regulates cell-identity-specific CD36 expression69. This H3K4me1 site is close to the most abundant CD36 promoter. Most of the enzymes that modify chromatin depend on intermediary metabolites functioning as substrates or cofactors, which helps explain why metabolism is critical for cellular renewal and differentiation after injury70. Thus, reduction in CD36-mediated FA metabolism would impair the chromatin modification needed for PC progenitor differentiation to PC and mucosal renewal (Fig. 9).
Data in rodents link CD36 to intestinal function and barrier integrity24,25 and this study presents evidence of its important role in stomach tissue repair. Appropriate repair is required to prevent gastritis, ulcers, hemorrhage, and the development of metaplasia14. The CD36 gene is polymorphic and CD36 variants associate with abnormal lipid metabolism57 and risk of cardiometabolic diseases71,72. Our findings in mice and biomedical databases support the contribution of CD36 variants to human gastrointestinal disorders. An estimated 11% of the US population suffer from a chronic digestive ailment, with prevalence reaching 35% for those 65 years and older and resulting in substantial morbidity, mortality, and cost73.
Methods
Animals
All protocols were approved by Washington University animal ethics committee. Mice housed in a 12 h light-dark facility were fed chow ad libitum (Purina) or 12 h fasted. Parietal cell Cd36 deficiency (PC-Cd36−/−) was obtained by crossing Cd36 floxed (Fl/Fl) mice with mice expressing the H+-K+-ATPase β (Atp4b) Cre. Cd36 deletion in endothelial cells (EC-Cd36−/−) used Tie2 Cre mice24,46. Cre+ males were bred to Cre– females to avoid germline transmission. Genotypes were confirmed by PCR and immunohistochemistry. All studies used C57Bl6, sex-matched mice cohorts.
Plasma hormones
Plasma gastrin in 12 h fasted and 4 h refed mice was assayed by ELISA (RayBio). Leptin was measured in 12 h fasted and 4 h refed mice, and in the vagus-dependent pre-absorptive phase from plasma collected at 0 and 15 min after oral fat exposure using Milliplex mouse metabolic hormone magnetic bead panel (Millipore Sigma).
High-resolution respirometry
Isolated corpus mucosa from WT and Cd36−/− mice (n = 4/genotype) was permeabilized (50 µg/mL saponin, 30 min, 4 °C), washed (10 min, 4 °C) in Mir05 respiration buffer, blotted, microbalance weighed, and transferred in fresh Mir05 with 3 mg/mL creatinine to the Oxygraph-O2k (Oroboros) chamber. Non-phosphorylative “Leak” was measured in presence of malate (1 mM), glutamate (10 mM) and pyruvate (5 mM). Oxygen consumption in the oxidative phosphorylation state (OxPHOS) was assayed by adding ADP (5 mM) and succinate (10 mM) and maximum flux (ETS) by uncoupling with FCCP. Assays were in duplicate.
Metabolomics and lipidomics
Metabolites (including acetylcholine and acylcarnitines) and lipids were analyzed using liquid chromatography-tandem mass spectrometry as described74 using the methanol/methyl tert-butyl ether/water extraction protocol75. Extracts were processed for lipidomic or metabolomic profiling.
Fatty acid uptake
Mice (12 h fasted, n = 6–7/genotype) were injected retro-orbitally with 100 µL PBS containing 2 µCi of [3H]oleic acid (Perkin Elmer) and perfused with 10 mL PBS through the left ventricle 5 min after injection. Excised tissues were homogenized in 500 µL PBS and aliquots (100 µL) added to 5 mL scintillation fluid (Optiphase HiSafe 3, Perkin Elmer) for radioactivity measurement. Tissue FA uptake was adjusted by tissue weight and by antrum radioactivity which did not differ between groups.
High-dose tamoxifen injury
Tamoxifen treatment was as previously42. Tamoxifen (TAM) was injected intraperitoneally daily for 3 days (250 mg/kg). Stomachs were collected at day 1 or 5 postinjection and from untreated mice for immunofluorescence. For quantification of injury and recovery gastric sections from control and tamoxifen (TAM) treated mice, were processed for immunofluorescence and at least five images with 10 well-oriented gastric units were obtained per stomach. Parietal cells were immunostained for ezrin and VEGFB and proliferating cells for Ki67. Chief cells were co-stained with the neck cell marker Griffonia Simplicifolia Lectin II (GSII), referred to as spasmolytic polypeptide (TFF2) expressing metaplasia (SPEM) cells). Parietal cell number and diameter were quantified by ImageJ software and proliferating (Ki67+), GIF+/GSII+ SPEM cells and PCs per gland unit were averaged for all units counted.
Histology
Stomachs were fixed in 10% formalin, and paraffin embedded76. Sections (5 μm) deparaffinized, treated (99 °C, 18 min) for antigen retrieval (rodent decloaker, Biocare Medical) were blocked 1 h in 1% donkey serum (Jackson Labs), 1% BSA (Sigma-Aldrich) and 0.3% Triton-X100. Primary antibodies (overnight, 4 °C) were followed by horseradish peroxidase (Jackson Immuno Research Labs) or fluorescently labeled secondary antibodies (Alexa Fluor 488 and 594; Invitrogen). Supplementary Table 1 lists primary antibodies and dilutions. Fluorescence used a Zeiss Axiovert 200 microscope with Axiocam MRM camera and Axiovision software. Bright-field images used a 2.0 HT NanoZoomer (Hamamatsu) whole slide scanner or an Olympus BX43 light microscope.
Electron microscopy
Stomachs, fixed overnight at 4 °C in modified Karnovsky’s buffer, were sectioned into rings and processed for EM. Mitochondrial morphology was evaluated using ImageJ software (> 50 mitochondria/cell).
Gene expression
Total RNA, isolated with TRIzol (Invitrogen) from frozen stomachs (n = 5-6/genotype) was reverse transcribed (ABI Prim 7000 Sequence Detection System; Applied Biosystems). Quantitative real-time PCR used Power SYBR Green Master Mix and 7500 Fast Real-Time PCR System (Applied Biosystems). Relative mRNA content (housekeeping gene 36B4) used δCt calculations (primers in Supplementary Table 2).
Western blotting
Tissue proteins separated by SDS-PAGE (4–12% acrylamide; Invitrogen), transferred to polyvinlyidene fluoride membranes (Millipore) and blocked (Li-COR Biosciences, Lincoln, NE), were incubated overnight (4 °C) with primary antibodies; mouse anti-mouse β-actin (1:5000), intrinsic factor (1:1000) (Santa Cruz Biotech), goat anti-mouse CD36 (1:1000, R&D Systems). Infrared dye-labeled secondary antibodies were added (1 h, room temperature) and signal detected (Li-Cor Odyssey Infrared) and adjusted to β-actin and total protein (Revert protein stain kit, Li-COR).
Statistics and reproducibility
Statistical analyses were performed using GraphPad Prism (V9; La Jolla CA). All data are means ± SEM. Two-way ANOVA followed by post hoc tests by Sidak multiple comparisons were used throughout, except as noted. Log-transformed metabolomic and lipidomic data were analyzed for effects of genotype, fasting, refeeding by two-way ANOVA using MetaboAnalyst 4.0 (FDR: 0.05) or in select cases using Prism 9. All statistical tests were two sided, with a P value of 0.05 considered statistically significant and P < 0.10 indicating a trend.
PrediXcan analysis
PrediXcan77 was used to evaluate CD36 contribution to the etiology of gastric disorders. The genetically determined expression component was estimated using gene expression imputation trained with reference transcriptome data (v6) from the Genotype-Tissue Expression (GTEx) Consortium52,53. PrediXcan was applied to patients of European ancestry with electronic health records tied to whole-genome genetic information in the BioVU resource of Vanderbilt University’s54. Table 1 lists the number of cases and controls for each trait. PrediXcan analysis on BioVU data was deemed non-human subjects research by VUMC IRB# 151187.
Reporting Summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
Source data files, including uncropped blots, are provided with this paper (Supplementary Data 1) and all other relevant data can be obtained from the corresponding author Miriam Jacome-Sosa upon reasonable request.
References
Schubert, M. L. Gastric acid secretion. Curr. Opin. Gastroenterol. 32, 452–460I (2016).
Churm, R., Davies, J. S., Stephens, J. W. & Prior, S. L. Ghrelin function in human obesity and type 2 diabetes: a concise review. Obes. Rev. 18, 140–148I (2017).
Lv, Y., Liang, T., Wang, G. & Li, Z. Ghrelin, a gastrointestinal hormone, regulates energy balance and lipid metabolism. Biosci. Rep. 38, BSR20181061 (2018).
Virdis, A. et al. Human Ghrelin: A Gastric Hormone with Cardiovascular Properties. Curr. Pharm. Des. 22, 52–58I (2016).
Cammisotto, P. & Bendayan, M. A review on gastric leptin: the exocrine secretion of a gastric hormone. Anat. Cell Biol. 45, 1–16I (2012).
Sobhani, I. et al. Vagal stimulation rapidly increases leptin secretion in human stomach. Gastroenterology 122, 259–263I (2002).
Hardwick, J. C., Van Den Brink, G. R., Offerhaus, G. J., Van Deventer, S. J. & Peppelenbosch, M. P. Leptin is a growth factor for colonic epithelial cells. Gastroenterology 121, 79–90I (2001).
Meek, T. H. & Morton, G. J. The role of leptin in diabetes: metabolic effects. Diabetologia 59, 928–932I (2016).
Yarandi, S. S., Hebbar, G., Sauer, C. G., Cole, C. R. & Ziegler, T. R. Diverse roles of leptin in the gastrointestinal tract: modulation of motility, absorption, growth, and inflammation. Nutrition 27, 269–275I (2011).
Schubert, M. L. & Rehfeld, J. F. Gastric peptides-gastrin and somatostatin. Compr. Physiol. 10, 197–228I (2019).
Green, R. et al. Vitamin B(12) deficiency. Nat. Rev. Dis. Prim. 3, 17040I (2017).
Yeomans, N. D. & Skeljo, M. V. Repair and healing of established gastric mucosal injury. J. Clin. Gastroenterol. 13(Suppl 1), S37–41I (1991).
Aihara, E. et al. Epithelial Regeneration After Gastric Ulceration Causes Prolonged Cell-Type Alterations. Cell. Mol. Gastroenterol. Hepatol. 2, 625–647I (2016).
Meyer, A. R. & Goldenring, J. R. Injury, repair, inflammation and metaplasia in the stomach. J. Physiol. 596, 3861–3867I (2018).
Wong, B. W. et al. The role of fatty acid beta-oxidation in lymphangiogenesis. Nature 542, 49–54I (2017).
Xiong, J. et al. A metabolic basis for endothelial-to-mesenchymal transition. Mol. Cell 69, 689–698 (2018). e687I.
Efeyan, A., Comb, W. C. & Sabatini, D. M. Nutrient-sensing mechanisms and pathways. Nature 517, 302–310I (2015).
Mihaylova, M. M. et al. Fasting activates fatty acid oxidation to enhance intestinal stem cell function during homeostasis and aging. cell stem cell 22, 769–778 (2018). e764I.
Chen, L. et al. HNF4 Regulates Fatty Acid Oxidation and Is Required for Renewal of Intestinal Stem Cells in Mice. Gastroenterology 158, 985–999 (2020). e989I.
Chen, M., Yang, Y., Braunstein, E., Georgeson, K. E. & Harmon, C. M. Gut expression and regulation of FAT/CD36: possible role in fatty acid transport in rat enterocytes. Am. J. Physiol. Endocrinol. Metab. 281, E916–923I (2001).
Mills, J. C. et al. A molecular profile of the mouse gastric parietal cell with and without exposure to Helicobacter pylori. Proc. Natl Acad. Sci. USA 98, 13687–13692I (2001).
Samovski, D. et al. Regulation of AMPK activation by CD36 links fatty acid uptake to beta-oxidation. Diabetes 64, 353–359I (2015).
Canton, J., Neculai, D. & Grinstein, S. Scavenger receptors in homeostasis and immunity. Nat. Rev. Immunol. 13, 621–634I (2013).
Cifarelli, V. et al. CD36 deficiency impairs the small intestinal barrier and induces subclinical inflammation in mice. Cell. Mol. Gastroenterol. Hepatol. 3, 82–98I (2017).
Abumrad, N. A. & Davidson, N. O. Role of the gut in lipid homeostasis. Physiol. Rev. 92, 1061–1085I (2012).
Sundaresan, S. et al. CD36-dependent signaling mediates fatty acid-induced gut release of secretin and cholecystokinin. Faseb j. 27, 1191–1202I (2013).
Tran, T. T. et al. Luminal lipid regulates CD36 levels and downstream signaling to stimulate chylomicron synthesis. J. Biol. Chem. 286, 25201–25210I (2011).
Lo, H. G. et al. A single transcription factor is sufficient to induce and maintain secretory cell architecture. Genes Dev. 31, 154–171I (2017).
Capoccia, B. J., Huh, W. J. & Mills, J. C. How form follows functional genomics: gene expression profiling gastric epithelial cells with a particular discourse on the parietal cell. Physiol. Genomics 37, 67–78I (2009).
Poirier, H., Degrace, P., Niot, I., Bernard, A. & Besnard, P. Localization and regulation of the putative membrane fatty-acid transporter (FAT) in the small intestine. Comparison with fatty acid-binding proteins (FABP). Eur. J. Biochem 238, 368–373I (1996).
Cammisotto, P. G. & Bendayan, M. Leptin secretion by white adipose tissue and gastric mucosa. Histol. Histopathol. 22, 199–210I (2007).
Bado, A. et al. The stomach is a source of leptin. Nature 394, 790–793I (1998).
Cinti, S. et al. Secretory granules of endocrine and chief cells of human stomach mucosa contain leptin. Int J. Obes. Relat. Metab. Disord. 24, 789–793I (2000).
Sobhani, I. et al. Leptin secretion and leptin receptor in the human stomach. Gut 47, 178–183I (2000).
Besnard, P. Lipids and obesity: Also a matter of taste? Rev. Endocr. Metab. Disord. 17, 159–170I (2016).
Browning, K. N. & Travagli, R. A. Central nervous system control of gastrointestinal motility and secretion and modulation of gastrointestinal functions. Compr. Physiol. 4, 1339–1368I (2014).
Laugerette, F. et al. CD36 involvement in orosensory detection of dietary lipids, spontaneous fat preference, and digestive secretions. J. Clin. Investig. 115, 3177–3184I (2005).
Engevik, A. C., Kaji, I. & Goldenring, J. R. The Physiology of the Gastric Parietal Cell. Physiol. Rev. 100, 573–602I (2020).
Xie, G., Drachenberg, C., Yamada, M., Wess, J. & Raufman, J. P. Cholinergic agonist-induced pepsinogen secretion from murine gastric chief cells is mediated by M1 and M3 muscarinic receptors. Am. J. Physiol. Gastrointest. Liver Physiol. 289, G521–529I (2005).
Takeuchi, K., Endoh, T., Hayashi, S. & Aihara, T. Activation of Muscarinic Acetylcholine Receptor Subtype 4 Is Essential for Cholinergic Stimulation of Gastric Acid Secretion: Relation to D Cell/Somatostatin. Front Pharm. 7, 278I (2016).
Huh, W. J. et al. Tamoxifen induces rapid, reversible atrophy, and metaplasia in mouse stomach. Gastroenterology 142, 21–24 (2012). e27I.
Saenz, J. B., Burclaff, J. & Mills, J. C. Modeling Murine Gastric Metaplasia Through Tamoxifen-Induced Acute Parietal Cell Loss. Methods Mol. Biol. 1422, 329–339I (2016).
Nomura, S. et al. Spasmolytic polypeptide expressing metaplasia to preneoplasia in H. felis-infected mice. Gastroenterology 127, 582–594I (2004).
Beyaz, S. et al. High-fat diet enhances stemness and tumorigenicity of intestinal progenitors. Nature 531, 53–58I (2016).
Knobloch, M. et al. A Fatty Acid Oxidation-Dependent Metabolic Shift Regulates Adult Neural Stem Cell Activity. Cell Rep. 20, 2144–2155I (2017).
Son, N. H. et al. Endothelial cell CD36 optimizes tissue fatty acid uptake. The. J. Clin. Investig. 128, 4329–4342I (2018).
Miller, M. J., Cusmano-Ozog, K., Oglesbee, D. & Young, S. Laboratory analysis of acylcarnitines, 2020 update: a technical standard of the American College of Medical Genetics and Genomics (ACMG). Genet Med. 23, 249–258 (2020).
Koves, T. R. et al. Mitochondrial overload and incomplete fatty acid oxidation contribute to skeletal muscle insulin resistance. Cell Metab. 7, 45–56I (2008).
Lee, H. J., Mayette, J., Rapoport, S. I. & Bazinet, R. P. Selective remodeling of cardiolipin fatty acids in the aged rat heart. Lipids Health Dis. 5, 2I (2006).
Han, X. et al. Alterations in myocardial cardiolipin content and composition occur at the very earliest stages of diabetes: a shotgun lipidomics study. Biochemistry 46, 6417–6428I (2007).
Nardone, G., Laccetti, P., Civiletti, C. & Budillon, G. Phospholipid composition of human gastric mucosa: a study of endoscopic biopsy specimens. Gut 34, 456–460I (1993).
Gamazon, E. R. et al. Using an atlas of gene regulation across 44 human tissues to inform complex disease- and trait-associated variation. Nat. Genet 50, 956–967I (2018).
Battle, A., Brown, C. D., Engelhardt, B. E. & Montgomery, S. B. Genetic effects on gene expression across human tissues. Nature 550, 204–213I (2017).
Unlu, G. et al. Phenome-based approach identifies RIC1-linked Mendelian syndrome through zebrafish models, biobank associations and clinical studies. Nat. Med 26, 98–109I (2020).
Bycroft, C. et al. The UK Biobank resource with deep phenotyping and genomic data. Nature 562, 203–209I (2018).
Kundaje, A. et al. Integrative analysis of 111 reference human epigenomes. Nature 518, 317–330I (2015).
Love-Gregory, L. et al. Higher chylomicron remnants and LDL particle numbers associate with CD36 SNPs and DNA methylation sites that reduce CD36. J. Lipid Res 57, 2176–2184I (2016).
Allen, L. H. et al. Biomarkers of Nutrition for Development (BOND): Vitamin B-12 Review. J. Nutr. 148, 1995s–2027sI (2018).
Haruma, K. et al. Old and New Gut Hormone, Gastrin and Acid Suppressive Therapy. Digestion 97, 340–344I (2018).
Dimaline, R. & Varro, A. Novel roles of gastrin. J. Physiol. 592, 2951–2958I (2014).
Hacioglu, A., Algin, C., Pasaoglu, O., Pasaoglu, E. & Kanbak, G. Protective effect of leptin against ischemia-reperfusion injury in the rat small intestine. BMC Gastroenterol. 5, 37I (2005).
Adeyemi, E. O. et al. Mechanisms of action of leptin in preventing gastric ulcer. World J. Gastroenterol. 11, 4154–4160I (2005).
McFarlan, J. T. et al. In vivo, fatty acid translocase (CD36) critically regulates skeletal muscle fuel selection, exercise performance, and training-induced adaptation of fatty acid oxidation. J. Biol. Chem. 287, 23502–23516I (2012).
Yoshida, Y. et al. Exercise- and training-induced upregulation of skeletal muscle fatty acid oxidation are not solely dependent on mitochondrial machinery and biogenesis. J. Physiol. 591, 4415–4426I (2013).
Nahlé, Z. et al. CD36-dependent regulation of muscle FoxO1 and PDK4 in the PPAR delta/beta-mediated adaptation to metabolic stress. J. Biol. Chem. 283, 14317–14326I (2008).
Willet, S. G. et al. Regenerative proliferation of differentiated cells by mTORC1-dependent paligenosis. EMBO J 37, e98311 (2018).
Harayama, T. & Shimizu, T. Roles of polyunsaturated fatty acids, from mediators to membranes. J. Lipid. Res. 61, 1150–1160I (2020).
Voelker, D. R. & Numata, M. Phospholipid regulation of innate immunity and respiratory viral infection. J. Biol. Chem. 294, 4282–4289I (2019).
Cui, K. et al. Chromatin signatures in multipotent human hematopoietic stem cells indicate the fate of bivalent genes during differentiation. cell stem cell 4, 80–93I (2009).
Sabari, B. R., Zhang, D., Allis, C. D. & Zhao, Y. Metabolic regulation of gene expression through histone acylations. Nat. Rev. Mol. Cell Biol. 18, 90–101I (2017).
Love-Gregory, L. et al. Variants in the CD36 gene associate with the metabolic syndrome and high-density lipoprotein cholesterol. Hum. Mol. Genet 17, 1695–1704I (2008).
Ma, X. et al. A common haplotype at the CD36 locus is associated with high free fatty acid levels and increased cardiovascular risk in Caucasians. Hum. Mol. Genet 13, 2197–2205I (2004).
Peery, A. F. et al. Burden of gastrointestinal disease in the United States: 2012 update. Gastroenterology 143, 1179–1187 (2012). e1173I.
Paluchova, V. et al. Lipokine 5-PAHSA Is Regulated by Adipose Triglyceride Lipase and Primes Adipocytes for De Novo Lipogenesis in Mice. Diabetes 69, 300–312I (2020).
Cajka, T., Smilowitz, J. T. & Fiehn, O. Validating Quantitative Untargeted Lipidomics Across Nine Liquid Chromatography-High-Resolution Mass Spectrometry Platforms. Anal. Chem. 89, 12360-–2368I (2017).
Ramsey, V. G. et al. The maturation of mucus-secreting gastric epithelial progenitors into digestive-enzyme secreting zymogenic cells requires Mist1. Development 134, 211–222I (2007).
Gamazon, E. R. et al. A gene-based association method for mapping traits using reference transcriptome data. Nat. Genet 47, 1091–1098I (2015).
Acknowledgements
We acknowledge assistance of the following facilities at Washington University: Nutrition and Obesity Research Center Cellular and Molecular Biology Core (NORC CMBC, P30 DK056341) with mitochondrial function and cytokine/hormone levels, the Hope Center Animal Surgery Core for pylorus ligation studies, the Hope Center Alafi Neuroimaging Laboratory (NIH Shared Instrumentation Grant S10-RR-027552) for Nanozoomer slide scanning and the Advanced Imaging and Tissue Analysis Core (AITAC, P30 DK052574) of the Digestive Disease Research Core Center (DDRC) for histology and microscopy. We acknowledge assistance of Karen Green at the Department of Pathology Electron Microscopy Center. We also acknowledge the Metabolomics Core Facility at the Physiology Institute of the Czech Academy of Sciences for lipidomics profiling. This work was supported by grants from the National Institute of Health DK060022 (NAA), DK060022S1 (MJS), DK094989, DK105129 (JCM), DK48370 and DK101332 (JRG), by NIH//NIA AG068026 and R01HG011138 (ERG) and a grant from Ministry of Education, Youth and Sports of the Czech Republic LTAUSA18104 (OK).
Author information
Authors and Affiliations
Contributions
M.J.S. designed experiments, obtained and analyzed data, and wrote the manuscript. Z.F.M., E.F.M., R.N., D.S., K.P., T.P., V.P., and H.G.L. helped with experiments and data analysis. AV conducted gastrin analysis, L.L.G. assisted with human data interpretation, J.R.G. contributed to data analysis and reviewed the manuscript, O.K. performed lipidomics and metabolomics and assisted with analyses, E.R.G. explored and analyzed human genetic data, J.C.M. contributed to experimental design, data analysis and reviewed the manuscript, N.A.A. designed experiments, analyzed data, and wrote the manuscript. M.J.S., J.C.M., and N.A.A. are guarantors of this work and, as such, had full access to all data and take responsibility for data integrity and accuracy of data analysis.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Communications Biology thanks the anonymous reviewers for their contribution to the peer review of this work. Primary Handling Editor: Eve Rogers. Peer reviewer reports are available.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jacome-Sosa, M., Miao, ZF., Peche, V.S. et al. CD36 maintains the gastric mucosa and associates with gastric disease. Commun Biol 4, 1247 (2021). https://doi.org/10.1038/s42003-021-02765-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s42003-021-02765-z
- Springer Nature Limited