Abstract
Introduction
Diarrhoea is a major public health concern in developing countries, usually exacerbated by poor water, sanitation and hygiene but its aetiology is under-studied, particularly away from capital cities. We identified diarrhoeagenic Escherichia coli (DEC) from stools collected in Ile-Ife and Ilesa, Osun state, Nigeria and determined their antibiotic resistance profiles.
Methods
Stool samples from 167 children with diarrhoea and 334 controls under the age of 5 years were cultured for Escherichia coli and Salmonella. Bacterial isolates were identified biochemically and DEC were identified by PCR. Antimicrobial susceptibility testing was by modified Kirby-Bauer disc diffusion method in accordance with the CLSI guidelines. Data were analyzed using Chi-square and Fisher’s exact tests.
Result
Diarrhoea infection is significantly high among children under 12 months (p = 0.002), caregivers without at least primary school education (p = 0.006), breastfeeding for under 6 months (p˂0.001), and caregivers who were siblings (p = 0.004). DEC was detected in 69(41.3%) cases but only 86(25.7%) controls (p < 0.001) and more commonly recovered during the wet season (p < 0.001). Enterotoxigenic E. coli (p = 0.031), enteropathogenic E. coli (p = 0.031) and Shiga-toxin-producing E. coli (p = 0.044) were recovered more commonly from cases than controls. DEC from patients with diarrhoea were commonly resistant to sulphonamides (91.3%), trimethoprim (82.6%), and ampicillin (78.3%) but were largely susceptible to quinolones and carbapenems (97.1%).
Conclusion
Enteropathogenic, enterotoxigenic and Shiga toxin-producing E. coli are associated with diarrhoea in our setting, and show considerable resistance to first-line antimicrobials. Risk factors for DEC diarrhoea include infancy, inadequate breastfeeding and caregivers with education below primary school.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Globally, diarrhoeal diseases are the second biggest cause of mortality for children under the age of five, accounting for one in nine child fatalities [1]. In resource-limited countries, Nigeria inclusive, diarrhoeal diseases are a major cause of morbidity [2,3,4] and diarrhoeagenic Escherichia coli (DEC) make an important but uncommonly qualified contribution to the problem [5]. The epidemiological significance of different DEC categories in childhood diarrhoea varies from one geographical area to another, and there are important regional differences in the prevalence of the different categories of DEC over time and seasons. In spite of these differences, few studies have been carried out in Africa to investigate the burden of the pathogens [4, 6,7,8].
Materials and methods
Study population
A total of 501 children aged between 0 and 60 months were recruited between October, 2016 and October, 2017 from primary, secondary, and tertiary hospitals (Enuwa Primary Health Center, Oke-Ogbo State Hospital Ile-Ife, Wesley Guild Hospital Ilesa, and Obafemi Awolowo University Teaching Hospitals Complex Ile-Ife) in Osun State, Nigeria, with a case and control proportion ratio of 1:2. This was calculated from Kelsey et al. [9] formula; \(n=\left(\frac{r+1}{r}\right) \frac{(\bar{p})(1-\bar{p})\left(Z_\beta+Z_{\alpha / 2}\right)^2}{\left(p_1-p_2\right)^2}\){where n= Sample size, Zα/2=0.84 (for 80% power), Zβ=1.96 (for 0.05 significance level), r= 2, p1= proportion exposed in the control group 24.9% Onanuga et al. [6], p2= Prevalence of DEC 37.1% Okeke et al. [7], with a 10% attrition rate}. Diarrhoea cases were children less than 5 years old that experienced three or more loose stools within 24-hours, while controls were children without diarrhoea visiting the same healthcare facility during the study period.
Specimen collection and processing
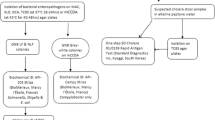
Using clean, sterile, and leak-proof universal bottles, fresh stool samples were collected from diarrhoea children (under five-year-olds) as well as age-matched, apparently healthy counterparts. All fresh stool samples of participants were inoculated into Selenite F broth, and on Eosin Methylene Blue agar and MacConkey agar plates (Oxoid Ltd., Hampshire, England) and incubated aerobically for 24 h at 37ºC. Following aseptic sub-culturing from Selenite F broth, plates of Salmonella Shigella Agar (SSA) were incubated aerobically at 37ºC for 24 h. Up to five distinct lactose-fermenting colonies were aseptically picked from Eosin Methylene Blue agar and MacConkey agar plates, streaked on Nutrient Agar (Oxoid Ltd., Basingstoke, Hampshire, England) and incubated aerobically at 37ºC for 24 h [10] and archived in a glycerol broth and stored in a freezer at -80°. The isolates were identified by conventional tube biochemical tests and confirmed with Microbact™ 24E identification kit (Oxoid Ltd., Basingstoke Hampshire, England). E. coli ATCC 25,922 served as the control strain.
Antimicrobial susceptibility testing
Antibiotic susceptibility testing against thirteen antimicrobials was performed using the modified Kirby-Bauer disc diffusion technique, following the guidelines set by the Clinical Laboratory Standards Institute [11]. The discs tested were ampicillin (10 µg), streptomycin (10 µg), trimethoprim (5 µg), tetracycline (30 µg), Nalidixic acid (30 µg), chloramphenicol (30 µg), ciprofloxacin (5 µg), sulphonamide (300 µg), cefotaxime (30 µg), ceftazidime (30 µg), cefoxitin (30 µg), amoxicillin-clavulanate (20/10µg) and ertapenem (10 µg) (Oxoid Ltd., Basingstoke Hampshire, England). E. coli ATCC 25,922 served as the control strain.
Detection of diarrhoeagenic E. coli virulence gene
DNA extraction was done using the Wizard Genomic DNA extraction Kit (Promega Corporation, Madison, USA) in accordance to manufacturer’s protocol [12] using aseptic precautions. A multiplex polymerase chain reaction (PCR) technique was used to screen all Escherichia coli for specific diarrhoea determinant genes [13]. The Multiplex PCR was grouped into PCR 1, PCR 2 and PCR 3 [13, 14]. Multiplex PCR assay 1 utilised three primer pairs and detected the presence of eae (Typical EPEC, atypical EPEC and EHEC are positive), bfpA (Only typical EPEC are positive, and target of CVD432 (typical EAEC are positive). Detection of ETEC, EHEC, STEC, EIEC and Shige PCR assay 2 used five primer pairs and detected the presence of LT and ST genes (ETEC are positive for one or both), stx1, stx2 (EHEC, STEC and Shigella dysentriae type 1 are positive for one or both), and ipaH (Shigella and EIEC are positive), generating PCR products of distinct sizes which were easily distinguished after agarose gel electrophoresis as presented in Table 1 [13]. PCR2 by Aranda et al. [13] seeks five targets. Two of these targets (180 bp) and (190 bp) are very close in size. To overcome the potential of failing to discriminate them in some reactions, in our laboratory, we have separated PCR2 into two reactions leaving us with PCR 3 [13], to detect ipaH (EIEC and Shigella), LT and ST (ETEC); PCR4 detects shiga-toxin 1 and 2 (STEC and EHEC).
Data analysis
Bivariate analysis of categorical variables was conducted using the Chi-Square test in Epi Info™ to evaluate the association between variables. When the expected frequency in any category was less than five, Fisher’s exact test was applied. Inferences were made based on the computed percentage positivity, 95% confidence intervals, and p-values. The level of significance was set at p˂ 0.05.
Results
A total of 501 children under the age of five were recruited over the study period (167 cases and 334 controls). Among the diarrhoea cases; there were 38 (22.8%) infants (less than 12 months), with 82 (49.1%) females and 85 (50.9%) males. As presented in Table 2, age < 12 months (38 [49%]), ϰ²(1) = 9.839, p = 0.002); caregivers with education below primary school (40 [46%]), ϰ²(1) = 7.574, p = 0.006); duration of breastfeeding < 6 months (21 [75%]), ϰ²(1) = 23.170, p < 0.001); and caregivers who were siblings (160 [78%]), ϰ²(1) = 8.146, p = 0.004), were significantly associated with diarrhoea.
Despite enrichment, Salmonella spp. was not recovered from any specimen in the study. A total of 618 E. coli isolates were obtained from the specimens. Out of these, PCR identified 256 as DEC, which originated from 155 unique individuals: 69 from cases and 86 from controls. DEC was recovered significantly more in cases, (69 [41.3%]), ϰ²(1) = 12.630, p < 0.001). As shown in Table 3, the most commonly detected DEC pathotype was enterotoxigenic E. coli (ETEC), which was recovered from 49 cases and 69 controls. Most of these ETEC strains 77 (65.3%) harboured the ST gene, encoding heat stable enterotoxin. Enteropathogenic E. coli isolates were recovered from 22 individuals and seven of these instances were typical EPEC, carrying the bfpA gene. All the specific DEC pathotypes sought, except EAEC and EIEC occurred significantly more in cases than controls: ETEC (49 [41.5%]), ϰ²(1) = 4.662, p = 0.031); EPEC (12 [54.5%]), ϰ²(1) = 4.659, p = 0.031); and STEC (4 [80.0%]), FE = 0.044, p = 0.044), as presented in Table 3.
Seasonal variation was observed in the occurrence of DEC in terms of number and pathotypes. The rate of recovery of DEC strains from children with diarrhoea was significantly higher in the wet season (March to October) (65 [94.2%]) in contrast to the dry season (4; 5.8%) (p < 0.001) as presented in Fig. 1.
Table 4 shows that among the diarrhoeal cases, there was high rates of resistance of the isolated DEC to commonly prescribed antibiotics, namely sulphonamide (63; 91.3%), trimethoprim (57; 82.6%), ampicillin (54; 78.3%) and tetracycline (40; 58.0%). By contrast, resistance to quinolones and carbapenems was uncommon (2.9%).
Discussion
Diarrhoeagenic Escherichia coli strains are pathogens of great public health importance, affecting both adults and children worldwide, but are infrequently sought because molecular or tissue culture methods are required to delineate them from commensals [6, 14]. While rotavirus often takes center stage as a leading cause of childhood diarrhoea, particularly in Africa, DEC strains, especially ETEC, EAEC, and EPEC, can contribute significantly to the overall burden [5, 14, 15]. The epidemiological significance of each DEC pathotypes in childhood diarrhoea varies from one geographical area to another [5]. Also, there are important regional differences in the prevalence of the different categories of DEC over time and seasons [5, 8, 14,15,16,17,18]. The prevalence of three DEC categories (ETEC, EAEC, and EPEC), was significantly higher in cases than in the controls (p˂0 001). Similar outcomes have also been reported in western (Ghana and Nigeria) [6, 19, 20] and south-eastern Africa (Mozambique) [21]. The fact that DEC was recovered from 23.7% of the controls in this study area shows that healthy children, who might act as reservoirs for transmission and/or suffer long term consequences of colonization [22], also harbour these pathogens. In this study, the five common pathotypes of E. coli—ETEC, EIEC, EPEC, EAEC, and STEC were identified; where ETEC, EPEC and STEC were significantly recovered more in diarrhoea cases than controls. This is consistent with the findings of other researchers from other developing countries, where the frequencies of recovery of ETEC [21, 23,24,25], EPEC [21], and STEC [23] were significantly higher in the cases than in the controls. Enterotoxigenic Escherichia coli (ETEC)-associated diarrhoea has been reported by many studies as the most common bacterial diarrhoea affecting children under 5 years old living in developing countries, as well as travellers to these countries [26]. In this study, ETEC was the most prevalent DEC pathotype, among both cases and controls, and was significantly associated with diarrhoea. This figure was comparable to findings from many [23, 27,28,29], but not all [6, 30, 31] other resource-limited countries. In addition, in a study on DEC among children with and without diarrhoea in Burkina Faso by Bonkoungou et al., ETEC was highly significantly associated with diarrhoea [32]. Altogether, reviews on DEC in sub-Saharan Africa stated that ETEC is associated with infantile diarrhoea in African countries and also the most common cause of acute diarrhoea [5, 33].
As in other studies, DEC were most predominantly recovered from children under one year of age [14, 8, 20, 25, 34, 35]. This age group represents a particularly vulnerable population to DEC infections due to factors such as immature immune systems and increased susceptibility to environmental pathogens [7, 14, 36]. Additionally, our study highlighted the significance of inadequate breastfeeding (less than 6 months) as another notable risk factor for DEC infection. This is comparable to what Ali et al. [37] and Akinlabi et al. [38] observed in northern and southwestern Nigeria. Breastfeeding provides infants with essential nutrients and antibodies that bolster their immune defences against infections, including DEC-related ones [14, 36,37,38]. Therefore, the absence or early cessation of breastfeeding may leave infants more susceptible to diarrhoeal illnesses, including those caused by DEC. Our finding and similar reports from elsewhere emphasize the importance of promoting exclusive breastfeeding for the first six months of life as an infectious diarrhoea prevention measure [38, 39].
Our study revealed a significant association between caregivers with a limited educational background and DEC infection. This finding underscores the multifactorial nature of diarrhoeal illnesses in children, highlighting the impact of socioeconomic factors on disease transmission [39, 40]. Caregivers with lower levels of education may have limited access to health education and resources, leading to suboptimal hygiene practices and increased susceptibility to DEC contamination in the household environment [39,40,41]. Our study also identified caregivers who are siblings as being associated with DEC infection among children. This suggests the potential contribution of intra-familial transmission routes in DEC spread. Siblings may facilitate close contact and shared exposure to contaminated environments, thereby increasing the risk of transmission within households [42].
This study revealed a seasonal variation in the prevalence of DEC infection in the environment. When compared to the dry season, the overall prevalence of DEC was shown to be significantly higher in the rainy season (p < 0.001). The peak prevalence of DEC (ETEC and EPEC) was observed in August, which is regarded as one of the months with the most rainfall in the study area, and is characterized by the contamination of surface waterways by sewage spills, faeces spills, and other waste spills. This finding is consistent with earlier research on the seasonal variation of DEC infection, including those by Onanuga et al., Tumwine et al., and El Metwally et al. [6, 43, 44].
Antimicrobial drug resistance in bacteria that cause diarrhoeal disease is a serious and growing problem [45]. Antimicrobials are not indicated for the treatment of most childhood diarrhoea diseases [46] but should be administered to children with invasive or protracted infections. Moreover, resistance in enteric isolates provides a picture of the gut reservoir of resistance genes, which can be transmitted to enteric organisms causing infections in other niches [14].
This study revealed high rates of antibiotic resistance among different DEC categories, in particular, resistance to sulphonamide, trimethoprim, amoxicillin clavulanic-acid, streptomycin, ampicillin and tetracycline, probably as a result of its increased availability of multiple generic formulations in the markets [8, 47] but also because mobile genes encoding resistance to these antimicrobials are often linked and transmitted together [14]. Substandard oral drugs, which are common in our setting [6, 14], often fail to be fully absorbed, leaving behind enough drug in the intestine to select for resistant enteric bacteria [48, 49]. Notably, the DEC isolates in this study remained susceptible to quinolones and carbapenems, highlighting the importance of preserving these critically-important antibiotics for severe infections [50]. Salmonella spp. was not recovered in this study despite enrichment and have been found uncommon in childhood diarrhoea studies performed in or close to our study area [6, 14, 38, 51]. As with some of those studies, we additionally did not identify any Shigella or many EIEC.
This study has several limitations. To begin with, controls were not time-matched with cases, possibly introducing temporal confounding. Secondly, only 1–2 isolates per specimen were screened for DEC by PCR. This limited screening might have affected our results, as typically screening 3–5 colonies can increase the yield of DEC, especially in children without diarrhoea who often carry multiple E. coli lineages. Akinlabi et al. [51] recently reported that the Aranda et al. [13] multiplex PCR protocol, which they compared with whole genome sequencing, had suboptimal sensitivity and specificity for certain DEC lineages that are common elsewhere in south western Nigeria. As we did not also identify DEC by whole genome sequencing, the degree to which this might affect our results is unclear. These limitations notwithstanding, the data point to a high incidence of DEC infections and a strong association with diarrhoea for multiple pathotypes. This highlights the need for more in-depth investigations using predictive tools in this study area, as well as further study of the isolates we obtained.
Conclusion
This study shows that DEC, particularly ETEC, EPEC, and STEC are important diarrhoeagenic agents in Ile-Ife and Ilesa, Nigeria. These findings highlight the need for routine surveillance and focused tool development against diarrhoeal disease. The prevalence of ETEC and EPEC, especially during the wet season, underscores the need for routine surveillance and targeted interventions to curb their spread. Notably, the study identified crucial risk factors like infancy, inadequate breast feeding and caregivers with education below primary school, emphasizing the importance of strengthening public health programs that promote optimal infant feeding practices, hygiene education, and safe water access. Furthermore, the substantial antibiotic resistance observed among DEC isolates necessitates the judicious use of antimicrobials and the exploration of alternative treatment strategies. By delving deeper into the specific virulence factors of prevalent DEC pathotypes and their environmental interactions, future research can pave the way for the development of effective diagnostics, and targeted interventions. This study not only contributes valuable knowledge to the fight against childhood diarrhoeal disease in Nigeria but also serves as a springboard for further research efforts aimed at protecting the health and well-being of vulnerable children, particularly those under five years of age, globally.
Data availability
The datasets used during the current study are available from the corresponding author (olayinkaademolaa@gmail.com) upon reasonable request.
Abbreviations
- E. coli :
-
Escherichia coli
- DEC:
-
Diarrhoeagenic E. coli
- CLSI:
-
Clinical Laboratory Standard Institute
- EPEC:
-
Enteropathogenic Escherichia coli
- ETEC:
-
Enterotoxigenic Escherichia coli
- EIEC:
-
Enteroinvasive Escherichia coli
- EAEC:
-
Enteroaggregative Escherichia coli
- EHEC / STEC:
-
Enterohemorrhagic (Shiga toxin- producing) Escherichia coli
- DAEC:
-
Diffusely adherent Escherichia coli
- STEC:
-
Shiga toxin producing E. coli
References
World Health Organization. (2023). Diarrhoeal disease. Retrieved January 21, 2023, from https://www.who.int/news-room/fact-sheets/detail/diarrhoeal-disease
Mokomane M, Kasvosve I, de Melo E, Pernica JM, Goldfarb DM. The global problem of childhood diarrhoeal diseases: emerging strategies in prevention and management. Therapeutic Adv Infect Disease. 2018;5(1):29–43.
UNICEF. (2020). Under five mortality. http://data.unicef.org/topic/child-survival/under-five-mortality/
Ugboko HU, Nwinyi OC, Oranusi SU, Fagbeminiyi FF. (2021). Risk factors of diarrhoea among children under five years in Southwest Nigeria. Int J Microbiol pp. 1–9.
Kotloff KL, Nasrin D, Blackwelder WC, Wu Y, Farag T, Panchalingham S, Sow SO, Sur D, Zaidi AKM, Faruque ASG, Saha D, Alonso PL, Tamboura B, Sanogo D, Onwuchekwa U, Manna B, Ramamurthy T, Kanungo S, Ahmed S, Qureshi S, Levine MM. The incidence, aetiology, and adverse clinical consequences of less severe diarrhoeal episodes among infants and children residing in low-income and middle-income countries: a 12-month case-control study as a follow-on to the global enteric Multicenter Study (GEMS). Lancet Global Health. 2019;7(5):e568–84.
Onanuga A, Igbeneghu O, Lamikanra A. A study of the prevalence of diarrhoeagenic Escherichia coli in children from Gwagwalada, Federal Capital, Nigeria. Pan Afr Med J. 2014;17:146.
Okeke IN, Lamikanra A, Steinruck H, Kaper JB. Characterization of Escherichia coli strains from cases of childhood diarrhoea in provincial southwestern Nigeria. J Clin Microbiol. 2000;38:7–12.
Opintan JA, Newman MJ, Arhin RE, Donkor ES. Laboratory- based nationwide surveillance of antimicrobial resistance in Ghana. Infect Drug Resist. 2015;54:191.
Kelsey JL, Whittemore AS, Evans AS, Thompson WD. Methods of sampling and estimation of sample size. In: Kelsey JL, Whittemore AS, Evans AS, Thompson WD, editors. Methods in Observational Epidemiology. New York: Oxford University Press; 1996.
Okeke I, Ojo O, Lamikanra A, Kaper J. Etiology of acute diarrhoea in adults in southwestern, Nigeria. J Clin Microbiol. 2003;41:4525–30.
Clinical and Laboratory Standards Institute (CLSI). (2024). Supplement M100: Performance Standards for Antimicrobial Susceptibility Testing. (L. L. Kristy and M. Laura, editors; 34th ed.).
Promega Corporation. Wizard genomic DNA purification kit Technical Manual. Madison, WI: Promega Corporation; 2019.
Aranda K, Fagundes-Neto U, Scaletsky I. Evaluation of multiplex PCRs for diagnosis of infection with diarrhoeagenic Escherichia coli and Shigella spp. J Clin Microbiol. 2004;42:5849–53.
Odetoyin BW, Hofmann J, Aboderin AO, Okeke IN. Diarrhoeagenic Escherichia coli in mother-child pairs in Ile-Ife, South Western Nigeria. BMC Infect Disease. 2015;16:28.
Rolande M, Mabika RM, Liabagui SL, Moundounga HK, Mounioko F, Souza A, Yala JF. Molecular prevalence and Epidemiological Characteristics of Diarrhoeagenic E. Coli in Children under 5 Years Old in the City of Koula-Moutou, East-Central Gabon. Open J Med Microbiol. 2021;11:157–75.
Ugboko HU, Nwinyi OC, Oranusi SU, Oyewale JO. (2020). Childhood diarrhoeal diseases in developing countries. Heliyon. 13;6(4):e03690.
Acosta GJ, Vigo NI, Durand D, Riveros M, Arango S, Zambruni M, Ochoa TJ. Diarrhoeagenic Escherichia coli: prevalence and pathotype distribution in children from Peruvian Rural communities. Am J Trop Med Hyg. 2016;95(3):574–9.
Ifeanyi CI, Ikeneche NF, Bassey BE, Al-Gallas N, Ben-Aissa R, Boudabous A. Diarrheagenic Escherichia coli pathotypes isolated from children with diarrhea in the Federal Capital Territory Abuja. Nigeria. J Infect Developing Ctries. 2015;19(2):165–74.
Addy PAK, Antepim G, Frimpong EH. Prevalence of pathogenic Escherichia coli and parasites in infants with diarrhoea in Kumasi, Ghana. East Afr Med J. 2004;81(7):353–7.
Saka HK, Dabo NT, Muhammad B, García-Soto S, Ugarte-Ruiz M, Alvarez J. Diarrheagenic Escherichia coli Pathotypes from children younger than 5 years in Kano State, Nigeria. Front Public Health. 2019;7:348.
Rappelli P, Folgosa E, Solinas ML. Pathogenic enteric Escherichia coli in children with and without diarrhoea in Maputo, Mozambique. FEMS Immunol Med Microbiol. 2005;43(1):67–72.
Kaper JB, Nataro JP, Mobley HL. (2004). Pathogenic Escherichia coli. Nature Reviews Microbiology. (2004) 2:123–40. 10.1038
Haghi F, Zeighami H, Hajiahmadi F, Khoshvaght H, Bayat M. Frequency and antimicrobial resistance of diarrhoeagenic Escherichia coli from young children in Iran. J Med Microbiol. 2014;63:427–32.
Vilchez S, Reyes D, Paniagua M, Bucardo F, Möllby R, Weintraub A. Prevalence of diarrhoeagenic Escherichia coli in children from León, Nicaragua. J Med Microbiol. 2009;58:630–7.
Prah I, Ayibieke A, Nguyen TTH, Iguchi A, Mahazu S, Sato W, Hayashi T, Yamaoka S, Suzuki T, Iwanaga S, Ablordey A, Saito R. Virulence profiles of Diarrheagenic Escherichia coli isolated from the Western Region of Ghana. Jpn J Infect Dis. 2020;24(2):115–21.
Levine MM, Kotloff KL, Nataro JP, Muhsen K. The global enteric Multicenter Study (GEMS): impetus, rationale, and genesis. Clin Infect Disease. 2012;55(Suppl 4):S215–24.
Okoh AI, Osode AN. Enterotoxigenic Escherichia coli (ETEC): a recurring decimal in infants’ and travelers’ diarrhoea. Rev Environ Health. 2008;23:135–48.
Qadri F, Ahmed A, Tarique A, Begum T, A. and, Svennerholm AM. Disease burden due to enterotoxigenic Escherichia coli in the first 2 years of life in an urban community in Bangladesh. Infect Immunol. 2007;75(8):3961–8.
Moyo SJ, Maselle SY, Matee MI, Langeland N, Mylvaganam H. Identification of diarrhoeagenic Escherichia coli isolated from infants and children in Dares Salaam, Tanzania. BioMed Cent Infect Disease. 2007;7:92.
Khairy RMM, Fathy ZA, Mahrous DM, Mohamed ES, Abdelrahim SS. Prevalence, phylogeny, and antimicrobial resistance of Escherichia coli pathotypes isolated from children less than 5 years old with community acquired- diarrhoea in Upper Egypt. BMC Infect Dis. 2020;1:20(1):908.
Zhou Y, Zhu X, Hou H, Lu Y, Yu J, Mao L, Mao L, Sun Z. Characteristics of diarrhoeagenic Escherichia coli among children under 5 years of age with acute diarrhoea: a hospital-based study. BMC Infect Dis. 2018;1:18(1):63.
Bonkoungou IJO, Lienemann T, Martikainen O, Dembele R, Sanou I, Traore AS, Siitonen A, Barro N, Haukka K. Diarrhoeagenic Escherichia coli detected by 16-plex PCR in children with and without diarrhoea in Burkina Faso. Clin Microbiol Infect. 2012;18:9.
Okeke IN. Diarrhoeagenic Escherichia coli in sub-saharan Africa: status, uncertainties and necessities. J Infect Developing Ctries. 2009;3(11):817–42.
Agho KE, Ezeh OK, Ghimire PR, Uchechukwu OL, Stevens GJ, Tannous WK, Fleming C, Ogbo FA. Global Maternal and Child Health Research collaboration (GloMACH). Exclusive Breastfeeding Rates and Associated Factors in 13 Economic Community of West African States (ECOWAS) Countries. Nutrients. 2019;11(12):3007.
Acosta GJ, Vigo NI, Durand D, Riveros M, Arango S, Zambruni M, Ochoa TJ. Diarrhoeagenic Escherichia coli: prevalence and pathotype distribution in children from Peruvian Rural communities. Am J Trop Med Hyg. 2016;7(3):574–9.
Egbontan AE, Ojo OA, Jacob SJ. Prevalence of Diarrhoea causing microorganisms among children that are exclusively breastfed and those on Weaning Foods. Pac J Sci Technol. 2013;14(1):334–41.
Ali M, Ahmed I, Yusha’u M, Shehu AA. (2023). Prevalence of Diarrhoea and Risk Associated factors among children under 5 years in Kano, North-western Nigeria. Archives Pharm Pharmacol Res. 3(3).
Akinlabi OC, Nwoko EQ, Dada RA, Ekpo S, Omotuyi A, Nwimo CC, et al. Epidemiology and risk factors for diarrheagenic escherichia coli carriage among children in Northern Ibadan, Nigeria. Am J Trop Med Hyg. 2023;109(6):1223–32.
Duche RT, Amali O, Umeh EU. Bacterial contamination of children’s Weaning foods in Asase, North Bank, Makurdi. Int J Sci Eng Res. 2013;4(8):2184–225.
Das R, Palit P, Haque MA, Ahmed T, Faruque ASG. Association between Pathogenic Variants of Diarrhoeagenic Escherichia coli and Growth in Children under 5 years of age in the global enteric Multicenter Study. Am J Trop Med Hyg. 2022;6(1071):72–81.
GebreSilasie YM, Tullu KD, Yeshanew AG. Resistance pattern and maternal knowledge, attitude and practices of suspected Diarrhoeagenic Escherichia coli among children under 5 years of age in Addis Ababa, Ethiopia: cross sectional study. Antimicrob Resist Infect Control. 2018;7:110.
Mattioli MC, Boehm AB, Davis J, Harris AR, Mrisho M. Enteric Pathogens in Stored Drinking Water and on Caregiver’s hands in Tanzanian households with and without reported cases of child diarrhoea. PLoS ONE. 2014;9(1):e84939.
Tumwine JK, Thompson J, Katua-Katua M, Mujwajuzi M, Johnstone N, Porras I. Diarrhoea and effects of different water sources, sanitation and hygiene behaviour in East Africa. Trop Med Int Health. 2002;7(9):750–6.
El Metwally HAR, Ibrahim HAH, El-Athamna MN, Amer MA. Multiplex PCR for detection of Diarrheagenic Escherichia coli in Egyptian Children. J Med Sci. 2007;7(2):255–62.
WHO (World Health Organisation). (2020). Global priority list of antibiotic-resistant bacteria to guide research, discovery, and development of new antibiotics. In World Health Organization (pp. 1–7).
Bruzzese E, Giannattasio A, Guarino A. Antibiotic treatment of acute gastroenteritis in children. F1000Research. 2018;15:7.
Von Baum H, Marre R. Antimicrobial resistance of Escherichia coli and therapeutic implications. Int J Med Microbiol. 2005;295:503–11.
Cavany S, Nanyonga S, Hauk C. The uncertain role of substandard and falsified medicines in the emergence and spread of antimicrobial resistance. Nat Commun. 2023;14:6153.
Holmes AH, Moore LS, Sundsfjord A, Steinbakk M, Regmi S, Karkey A, Guerin PJ, Piddock LJ. Understanding the mechanisms and drivers of antimicrobial resistance. Lancet. 2016;387:176–87.
Antimicrobial Resistance Collaborators. Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. Lancet. 2022;399:629–55.
Akinlabi OC, Dada RA, Nwoko EQA, Okeke IN. PCR diagnostics are insufficient for the detection of Diarrhoeagenic Escherichia coli in Ibadan, Nigeria. PLOS Global Public Health. 2023;7(8):e0001539.
Acknowledgements
We thank Dr. Olabisi C. Akinlabi for helpful suggestions and staff of the health facilities for assistance with enrolling and caring for participants.
Funding
This work was supported by African Research Leader’s Award MR/L00464X/1 (to I. N. O.), which was jointly funded by the United Kingdom Medical Research Council (MRC) and the United Kingdom Department for International Development (DFID) under the MRC/DFID Concordat agreement and is also part of the EDCTP2 program supported by the European Union. I. N. O. is a Calestous Juma Fellow supported by the Bill and Melinda Gates Foundation (Grant no. INV-036234).
Author information
Authors and Affiliations
Contributions
AOA and INO conceived this study and came up with the adapted methodology. AAO and IOO carried out the sample collection and performed the experiments. AAO and IOO carried out the data analysis and wrote the manuscript. AAO prepared all the tables and figures with the guidance of AOA and INO. Grants for this research are obtained by INO. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The study was approved by the ethics committee of the Obafemi Awolowo University Teaching Hospitals Complex, Ile-Ife (IRB/IEC/0004553; NHREC/27/02/2009a) and the University of Ibadan/University College Hospital ethics committee (UI/EC/15/0093). Parents or guardians of the children gave written informed consent and filled out a questionnaire to provide demographic data and the breastfeeding pattern for each child.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Olayinka, A.A., Oginni-Falajiki, I.O., Okeke, I.N. et al. Diarrhoeagenic Escherichia coli associated with childhood diarrhoea in Osun state, Nigeria. BMC Infect Dis 24, 928 (2024). https://doi.org/10.1186/s12879-024-09793-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12879-024-09793-0