Abstract
Background
Fahr’s disease is a very rare inherited neurodegenerative disorder characterized by diffuse and symetric intracranial calcification of the bilateral basal ganglia and cerebellum. Although the disease is slowly progressive, several acute forms have been described. We would like to present a very rare case of Fahr’s disease with an ischemic stroke and its hemorrhagic transformation.
Case presentation
A 70-year-old woman presented to our emergency department with rapid cognitive decline, dysarthria and right limb weakness. Cranial computed tomography showed diffuse and symmetric hyperdense areas at the level of the bilateral dentate nuclei of cerebellar hemispheres and basal ganglia, suggestive of calcification consistent with Fahr's disease on a background of thyroidectomy history, and effacement in the left caudate region. The patient was admitted to the intensive care unit with suspected left cerebral ischemic stroke. Because of clinical deterioration with increasing drowsiness and right hemiplegia, a control computed tomography scan was performed. Upon detection of a 6 * 8 cm lesion corresponding to an intracerebral hematoma in the left temporoparietal area with intraventricular component, she underwent surgery. The patient did not become hemodynamically stable and died on post-operative day 3.
Conclusions
The calcium deposits in the walls of the cerebral vessels in Fahr’s disease may exacerbate inflammatory processes leading to disruption of the blood-brain barrier. In addition, peripheral blood extravasation into the disrupted blood brain barrier due to ischemic stroke may lead to hemorrhagic transformation.
Similar content being viewed by others
Background
Fahr’s syndrome (idiopathic basal ganglia calcification) is a very rare inherited or sporadic neurodegenerative disorder characterized by diffuse and symetric intracranial calcification of the bilateral basal ganglia and cerebellum [1]. Fahr’s disease (FD) must be distinguished from Fahr’s syndrome, in which basal ganglia calcification is attributed to secondary cause in FD [2]. FD patients have different clinical presentations; they may be asymptomatic or present with a slowly progressive disorder, parkinsonism, chorea, dystonia, seizures, headache, or ataxia [3]. However, various acute manifestations have also been described: Epilepsy, syncope, ischemic stroke, and subarachnoid hemorrhage [4]. We would like to present a very rare case of FD with ischemic stroke and its hemorrhagic transformation.
Case presentation
A 70-year-old woman presented to our emergency department with rapid cognitive decline, dysarthria and right limb weakness. Her surgical history included thyroidectomy 9 years ago, aortic and mitral valve replacement 8 years ago. She had intermittent episodes of hypocalcemia after thyroidectomy. In addition, laboratory tests indicated characteristic hypoparathyroidism.
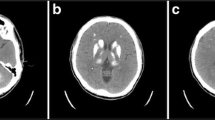
On neurological examination, she was cooperative with auditory stimuli and partially cooperative with simple commands. She was motor-weighted mixed aphasic. Left vulpian was positive. The right nasolabial groove was faint. Motor examination revealed right hemiparesis with manuel muscle strength grade 3. The National Institutes of Health Stroke Scale (NIHSS) score was sixteen. Magnetic resonance imaging could not be performed due to a history of heart valve replacement. Cranial computed tomography (CT) showed diffuse and symmetric hyperdense areas at the level of the bilateral dentate nuclei of cerebellar hemispheres (Fig. 1a) and basal ganglia (Fig. 1b), suggestive of calcification consistent with FD in the the histroy of thyroidectomy, and effacement in the left caudate region (Fig. 1c). The patient was admitted to the intensive care unit with suspected left ischemic stroke .
Control brain CT was performed on the 2nd day of hospitalization due to clinical deterioration in the context of increasing drowsiness and right hemiplegia. Upon detection of a 6 * 8 cm lesion corresponding to an intracerebral hematoma (ICH) in the left temporoparietal area with intraventricular component, she underwent surgery (Fig. 2). A left-sided temporo-parietal craniotomy with sylvian dissection was performed, and a gross-total resection was achieved by microsurgical techniques (Fig. 3). Histopathology showed fibrinoid necrosis and fibrinopurulent exudate infiltrated with dense active chronic inflammatory cells within bleeding areas, consistent with a hematoma. The patient did not become hemodynamically stable and died on the post-operative day 3.
Conclusions
Calcium deposition in the walls of cerebral vessels in FD may increase inflammatory processes leading to blood-brain barrier disruption. In addition, peripheral blood extravasation into the disrupted blood-brain barrier due to ischemic stroke may lead to hemorrhagic transformation [5]. The inflammatory relationship between hemorrhagic transformation and intracranial calcification deserves special attention and further investigation.
Availability of data and materials
Not applicable.
Abbreviations
- CT:
-
Computed tomography
- FD:
-
Fahr’s disease
- ICH:
-
Intracerebral hematoma
References
Mufaddel AA, Al-Hassani GA. Familial idiopathic basal ganglia calcification (Fahr’s disease). Neurosciences. 2014;19(3):171–7.
Pistacchi M, Gioulis M, Sanson F, Marsala SZ. Fahr’s syndrome and clinical correlation: a case series and literature review. Folia Neuropathol. 2016;54(3):282–94.
Donzuso G, Mostile G, Nicoletti A, Zappia M. Basal ganglia calcifications (Fahr’s syndrome): related conditions and clinical features. Neurol Sci. 2019;40(11):2251–63.
Sgulò FG, di Nuzzo G, de Notaris M, Seneca V, Catapano G. Cerebrovascular disorders and Fahr’s disease: report of two cases and literature review. J Clin Neurosci. 2018;50:163–4.
Mishra NK, Tsivgoulis G, Chen H, Spronk E, Sykes G, Falcione S, et al. Hemorrhagic transformation in ischemic stroke and the role of inflammation. Front Neurol [Internet]. 2021;1:661955.
Acknowledgements
Not applicable.
Funding
No funding.
Author information
Authors and Affiliations
Contributions
OB performed a literature research and analysis of originality of the case. The writing phase was done by OB. The author read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Written informed consent was obtained from the patient included in this study.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Başkurt, O. Hemorrhagic transformation of ischemic stroke in a patient with Fahr’s disease. Egypt J Neurosurg 38, 27 (2023). https://doi.org/10.1186/s41984-023-00207-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s41984-023-00207-y